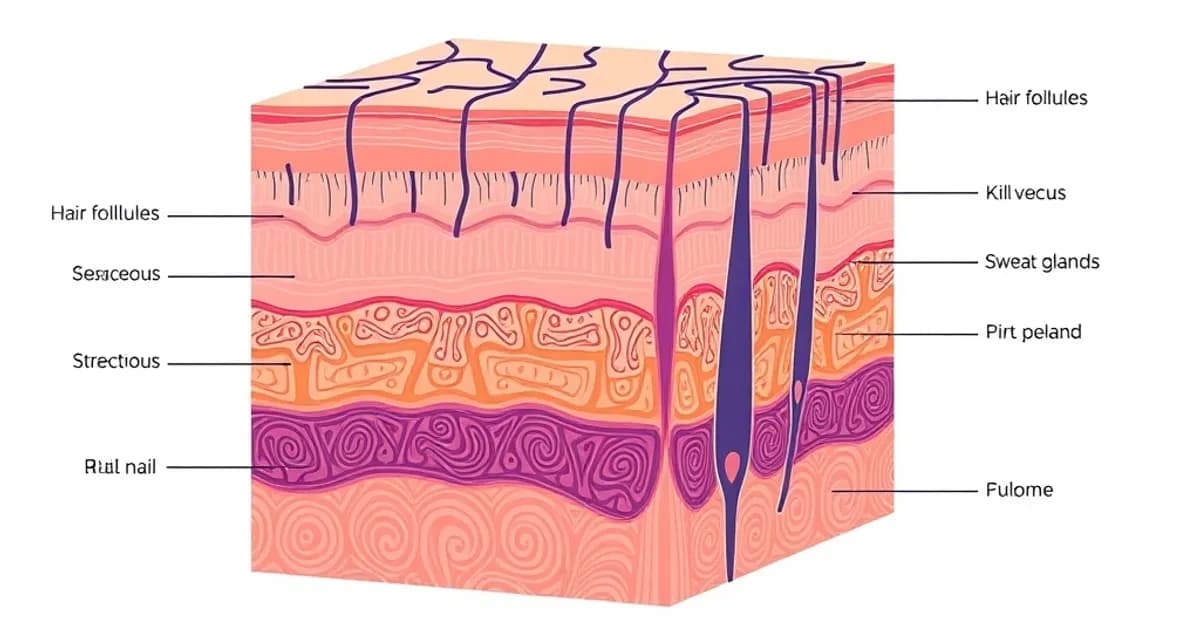
Hair Follicles and Hair Structure
Hair follicles are complex organs that produce hair, a distinctive mammalian feature. Each follicle extends from the epidermis deep into the dermis or hypodermis.
Key Follicle Components
The follicle structure includes multiple layers:
- Outer root sheath: Outermost protective layer
- Inner root sheath: Middle protective layer
- Hair shaft: The visible hair itself
- Hair bulb: Contains the hair matrix at the base
- Hair papilla: Supplies blood vessels and nerves to nourish growing cells
Three Phases of Hair Growth
Hair grows through distinct phases:
- Anagen (active growth): Lasts 2-7 years
- Catagen (transition): Lasts 2-3 weeks
- Telogen (resting): Lasts 2-3 months
After telogen, the hair sheds and the follicle begins anagen again.
Functions and Clinical Importance
The arrector pili muscle attaches to each follicle. It contracts in response to cold or emotional stimuli, creating the sensation of hair standing on end.
Hair serves multiple functions including insulation, UV protection, and sensory perception. Body regions have varying hair densities and types. Scalp follicles are most productive. Facial hair shows distinct growth patterns influenced by androgens.
Understanding follicle anatomy explains conditions like alopecia, folliculitis, and ingrown hairs.
Sebaceous Glands and Oil Secretion
Sebaceous glands are holocrine glands that produce sebum, an oily substance essential for skin and hair health. These glands distribute across the body in varying densities, with highest concentration on the face, scalp, and upper back.
Gland Structure and Development
Most sebaceous glands develop as outgrowths of hair follicles, forming pilosebaceous units. Some glands exist on non-hairy skin like lips and eyelids.
The gland structure consists of secretory acini surrounding a central duct. This duct empties into the hair follicle.
Sebum Production Process
Sebaceous gland cells undergo mitosis in the basal layer. They mature as they move toward the center. Cells accumulate lipid droplets and eventually rupture to release sebum through holocrine secretion.
Sebum Composition and Function
Sebum contains triglycerides, fatty acids, cholesterol, and cholesterol esters. This mixture creates a waterproof barrier protecting skin and hair.
Adults produce approximately 100-150 grams of sebum daily. Production varies based on hormonal status, genetics, and environmental factors.
Hormonal Control and Disorders
Androgens primarily control sebaceous gland activity. This explains why acne often develops during puberty when androgen levels surge.
Excessive sebum production contributes to acne development. Insufficient sebum causes dry skin conditions. Understanding this anatomy helps comprehend skin disorders and develop appropriate treatments.
Sweat Glands: Eccrine and Apocrine Types
The skin contains two distinct sweat gland types: eccrine and apocrine glands. Each has unique anatomy, distribution, and secretory products.
Eccrine Sweat Glands
Eccrine sweat glands are abundant across the entire body surface. They concentrate most on palms, soles, and forehead.
These glands have simple tubular structure:
- Secretory coil: Located in the hypodermis
- Straight duct: Passes through the dermis
- Terminal pore: Opens directly onto the skin surface
Eccrine glands produce watery sweat containing water, electrolytes (sodium chloride, potassium), and small amounts of urea and metabolic wastes.
This thermoregulatory sweating activates when body temperature increases. Sympathetic cholinergic innervation controls this response. Humans produce up to 1-2 liters of eccrine sweat per hour during intense heat or exercise.
Apocrine Sweat Glands
Apocrine sweat glands concentrate in specific regions:
- Axilla (underarm)
- Groin
- Anal region
- Areola of the breast
Apocrine glands are larger than eccrine glands. Their secretory coils sit deeper in the hypodermis. The duct opens into the hair follicle, not directly onto skin.
Apocrine secretion is thicker and oilier than eccrine sweat. It contains proteins, lipids, and steroids. Skin bacteria break down these compounds, producing body odor.
Functional Differences
Apocrine gland activity increases during emotional stress and sexual arousal. Temperature changes do NOT activate apocrine glands.
Understanding both gland types explains sweating patterns, body odor development, and conditions like hyperhidrosis and bromhidrosis.
Nails: Structure and Growth
Nails are specialized appendages made of tough, translucent protein matrix. They protect fingertips and provide mechanical advantage for fine motor tasks.
Key Nail Components
- Nail plate: Visible keratinized portion composed of multiple keratin-filled cell layers
- Nail bed: Contains melanocytes, abundant vasculature, and nerve endings beneath the plate
- Nail matrix: Germinal tissue under the proximal nail fold producing new cells through mitosis
- Nail groove: Anatomical channel anchoring lateral nail edges to surrounding skin
- Cuticle (eponychium): Fold of skin overlapping the nail base, providing pathogen protection
Growth Rates and Replacement
Normal fingernails grow approximately 0.1 millimeters per day. Complete replacement requires 4-6 months. Toenails grow more slowly, requiring 6-12 months for complete replacement.
Nail growth depends on age, nutritional status, hormonal factors, and overall health.
Normal Features and Abnormalities
Longitudinal ridges on healthy nails are normal and increase with age. Various abnormalities indicate systemic health conditions:
- Beau's lines: Horizontal depressions from illness
- Clubbing: Curved nails indicating respiratory disease
- Terry's nails: White appearance suggesting liver or kidney disease
- White spots: Indicate trauma or nutritional deficiency
Nail examination helps clinicians identify signs of nutritional deficiencies, infections, and systemic diseases.
Clinical Significance and Study Strategies
Skin appendages and glands are frequently affected by pathological conditions. Common disorders include acne vulgaris, alopecia, hyperhidrosis, and fungal or bacterial infections.
Understanding anatomical basis enables proper diagnosis and treatment selection.
Effective Study Strategies
Organize information by gland type and anatomical location rather than scattered facts. Create comparison flashcards that distinguish:
- Eccrine from apocrine glands
- Terminal hairs from vellus hairs
- Active growth from resting phases
Use anatomical diagrams and label major structures repeatedly. Include the pilosebaceous unit, hair bulb, hair papilla, sebaceous gland ducts, sweat gland coils, and nail components.
Why Flashcards Work Best
Flashcards excel for this topic because skin appendages require memorizing:
- Specialized terminology: Eccrine, apocrine, holocrine, follicle, matrix, papilla
- Functional relationships: How structure enables function
- Clinical applications: How anatomy explains disease
Retention Techniques
Space your studying across multiple sessions for spaced repetition, which strengthens long-term retention of anatomical details.
Create mnemonics for differences. Example: "Apocrine glands are in specific Areas. Eccrine glands are Everywhere."
Connect anatomy to physiology by understanding why structures are shaped as they are. Testing yourself regularly identifies weak areas requiring additional review.