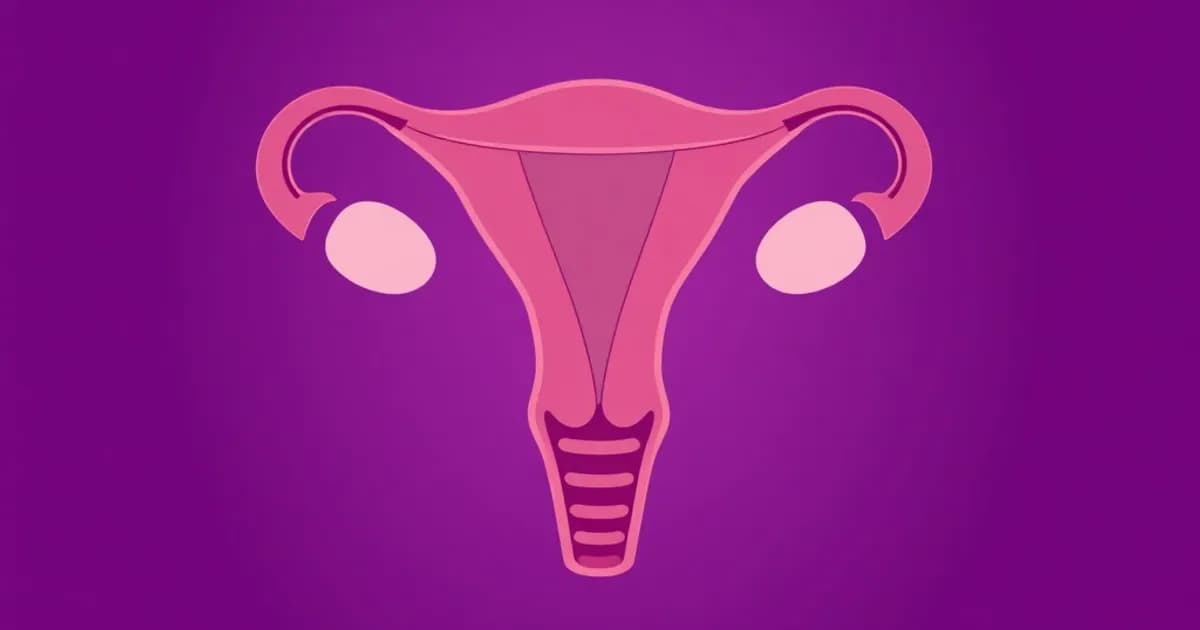
Gross Anatomy of the Uterus
The uterus is a hollow, muscular organ located in the pelvis. It sits between the bladder in front and the rectum behind. The organ measures approximately 7-8 centimeters long, 5-6 centimeters wide, and weighs 30-40 grams in non-pregnant women.
Three Main Regions
The uterus divides into three distinct regions. The fundus is the upper rounded portion above the uterine tubes. The body (corpus) is the central muscular section comprising about two-thirds of the organ. The cervix is the lower cylindrical portion.
The uterine cavity is normally only 1-2 millimeters wide when not distended. This potential space expands dramatically during pregnancy to accommodate the growing fetus. The uterus typically tilts forward over the bladder, a position called anteversion, though this varies among individuals.
Supporting Ligaments
Several ligaments support the uterus within the pelvis:
- Broad ligament - the largest supporting structure
- Round ligament - extends from fundus to labia majora
- Cardinal ligament - connects cervix to pelvic sidewall
- Uterosacral ligament - extends posteriorly to sacrum
The uterine tubes (fallopian tubes) extend laterally from the superior lateral angles where the fundus meets the body. Understanding the three-dimensional position and relationships of the uterus is crucial for studying gynecological procedures and pathology.
Histological Layers and the Cervix
The uterine wall consists of three distinct histological layers. Each layer has a specific structure and function in reproduction and menstruation.
Three-Layer Uterine Wall
The perimetrium is the outer serous covering, a continuation of visceral peritoneum. It covers the fundus and body but not the cervix. The myometrium is the thick muscular layer containing three indistinct layers of smooth muscle. The endometrium is the inner mucosal lining, highly dynamic and responsive to hormonal changes.
The myometrium's three layers are the outer longitudinal layer, middle circular layer with blood vessels and nerves, and inner longitudinal layer. During menstruation and labor, coordinated contractions of these muscles expel endometrial tissue and the fetus. The endometrium thickens during the proliferative phase (0.5-5 millimeters) and secretory phase, reaching up to 10 millimeters thickness. It consists of simple columnar epithelium, glands, and highly vascularized stromal tissue.
Cervical Structure and Function
The cervix is structurally distinct from the uterine body. It comprises primarily fibrous connective tissue with minimal smooth muscle. The cervical canal is lined with simple columnar epithelium that produces cervical mucus varying in consistency throughout the menstrual cycle.
The external cervical os opens into the vagina. The internal cervical os opens into the uterine cavity. The squamocolumnar junction is where stratified squamous epithelium of the vagina meets columnar epithelium of the cervix. This area is clinically significant as a common site for cervical cancers. Understanding these tissue layers explains menstrual physiology, pregnancy changes, and disease processes.
Blood Supply, Innervation, and Lymphatic Drainage
The uterus receives arterial blood supply primarily from the uterine arteries. These vessels branch from the internal iliac artery on each side and approach the uterus at the level of the internal cervical os.
Arterial Supply and Venous Drainage
The uterine arteries divide into ascending and descending branches that connect with the ovarian arteries above and vaginal arteries below. These vessels traverse through the cardinal ligaments and enter the uterus laterally. The ovarian vessels supply the fundus and upper uterine body. The vaginal branches supply the lower uterus and cervix. Venous drainage follows a similar pattern, with uterine veins draining into the internal iliac vein. This dual blood supply is clinically important during hysterectomy procedures.
Nerve Supply
The uterus receives sympathetic innervation from T12 and L1 spinal segments. Parasympathetic innervation comes from S2-S4 segments through the pelvic plexus. Sensory innervation from the cervix and lower uterus travels through pelvic splanchnic nerves. The fundus and upper body transmit pain sensation through ovarian nerve plexuses. This explains why dysmenorrhea pain is often felt in the lower abdomen and back.
Lymphatic Drainage Routes
Lymphatic drainage follows blood vessels throughout the pelvic region:
- Upper uterine body lymphatics drain to lumbar and aortic nodes
- Lower uterine body and cervical lymphatics drain to external iliac nodes
- Cervical lymphatics drain to internal iliac nodes
Understanding vascular and neural anatomy is essential for clinical procedures including epidural anesthesia, hysterectomy, and gynecological cancer treatment.
Cervical Anatomy and the Cervical Canal
The cervix is the lowermost portion of the uterus, measuring approximately 2-3 centimeters long and 2.5-3 centimeters in diameter. It extends from the internal cervical os proximally to the external cervical os distally, where it projects into the vagina.
Cervical Divisions and the Canal
The cervix divides into the supravaginal portion above the vaginal vault and vaginal portion extending into the vagina. The cervical canal is a spindle-shaped passage through which sperm must travel to reach the uterine cavity and fallopian tubes. Menstrual blood and uterine tissue are also expelled through this canal.
The cervical epithelium produces mucus from specialized glands called cervical crypts. During the follicular phase, estrogen stimulates thin, watery cervical mucus that allows sperm penetration. During the luteal phase, progesterone causes thick, viscous mucus forming a cervical plug preventing sperm entry. This mucus variation indicates fertility status.
Cervical Composition and Labor Changes
The cervix is fibrous with a small amount of smooth muscle from the uterine myometrium. Unlike the uterine body lined with endometrial tissue, the cervix is lined with columnar epithelium producing cervical mucus year-round. The cervical stroma contains numerous glands and is highly vascularized.
During labor, the cervix dilates from closed to approximately 10 centimeters. This remarkable stretching capacity allows passage of the fetus. The cervix is susceptible to various pathologies including cervicitis, polyps, and cervical cancer. Its anatomy is crucial for gynecological examination and screening.
Cyclical Changes and Clinical Significance
The endometrium undergoes dramatic cyclic changes during the 28-day menstrual cycle. Hormonal fluctuations drive these changes in preparation for implantation or menstruation.
Menstrual Cycle Phases
During the proliferative phase (days 1-14), rising estrogen levels stimulate endometrial growth and glandular development. The endometrium thickens from approximately 0.5 millimeters to 5-10 millimeters. Following ovulation, the secretory phase (days 15-28) begins as progesterone from the corpus luteum promotes glandular differentiation and increased vascularization.
If fertilization does not occur, declining progesterone levels trigger menstruation. The functional layer of the endometrium sheds through uterine contractions. Understanding these normal cyclic changes helps recognize abnormal patterns like dysmenorrhea (painful periods), menorrhagia (heavy bleeding), and amenorrhea (absent periods).
Cervical Cycle Changes
The cervix also undergoes cyclic changes. During the follicular phase, increased estrogen makes cervical mucus thin and stretchy. This facilitates sperm transport. Progesterone in the luteal phase causes cervical mucus to become thick and cellular, creating a barrier to sperm.
Common Pathologies
The cervix and uterus are common sites of pathology:
- Fibroids - benign smooth muscle tumors
- Endometrial cancer - malignant growth in endometrial tissue
- Cervical cancer - often related to human papillomavirus (HPV) infection
- Endometriosis - growth of endometrial tissue outside the uterus
Cervical cancer risk increases significantly with HPV infection. Regular cervical screening through Pap smears and HPV testing is crucial for women's health. The cervix's role as a barrier between the sterile uterine cavity and contaminated vaginal environment is clinically significant. Cervical incompetence can lead to recurrent miscarriage. Knowledge of normal anatomy is the foundation for understanding these pathological conditions and their clinical management.