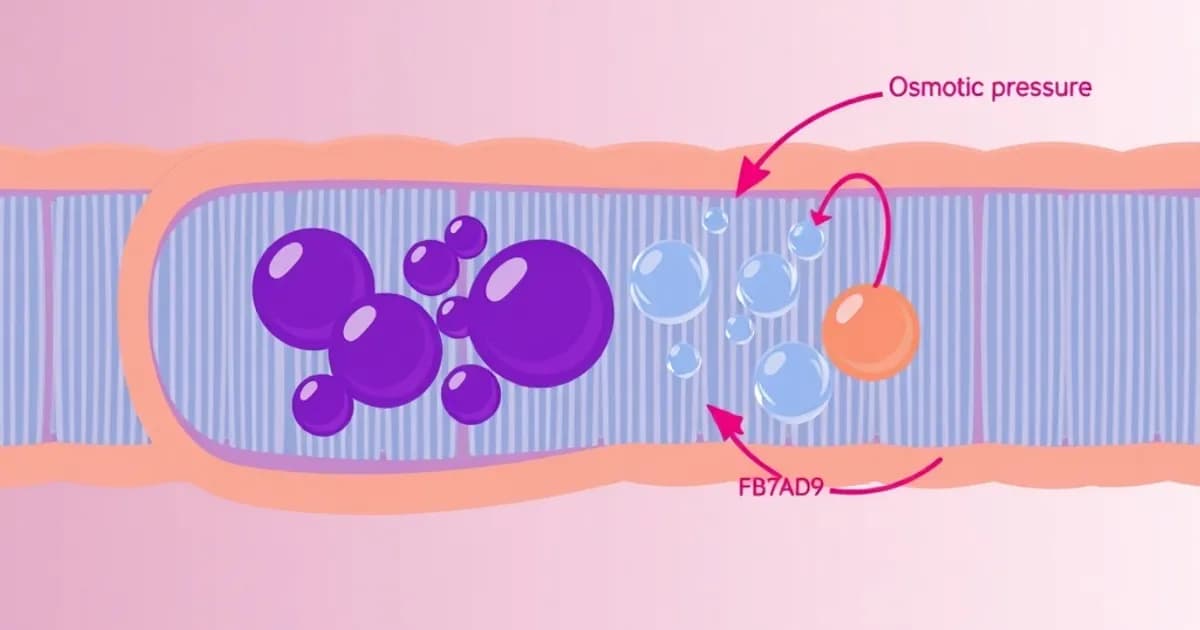
Mechanism of Action of Osmotic Diuretics
How Osmotic Diuretics Create Diuresis
Osmotic diuretics function through a fundamentally different mechanism than loop or thiazide diuretics. These agents increase osmotic pressure within the renal tubule lumen, which prevents water reabsorption in the proximal tubule and descending loop of Henle.
When mannitol or sorbitol is filtered by the glomerulus, the tubular epithelium cannot reabsorb it. This creates an osmotic gradient that draws water into the tubular lumen. The increased fluid volume leads to decreased sodium reabsorption because fluid moves through the tubule too quickly for normal reabsorption.
Key Difference from Other Diuretics
Unlike other diuretics, osmotic agents do not directly inhibit sodium pumps or channels. They work through passive osmotic forces instead. This distinction is crucial for understanding why they work even in severely compromised kidneys.
Mannitol vs. Sorbitol: Chemical Properties
Mannitol is a six-carbon sugar alcohol and the most commonly used osmotic diuretic clinically. Sorbitol is another sugar alcohol but is used less frequently due to metabolic complications.
Both agents are freely filtered at the glomerulus and minimally reabsorbed, making them ideal for creating sustained osmotic gradients. The diuretic effect is relatively rapid, occurring within 30-60 minutes of administration. The duration typically lasts 4-6 hours.
Understanding this mechanism explains why osmotic diuretics are effective regardless of the underlying cause of edema or fluid overload.
Clinical Applications and Indications
Cerebral Edema and Brain Injury
The most critical indication for mannitol is cerebral edema. Mannitol rapidly draws fluid from the interstitial and intracellular spaces of the brain into the bloodstream, reducing intracranial pressure. This makes mannitol invaluable in cases of:
- Traumatic brain injury
- Hemorrhagic stroke
- Post-neurosurgical procedures
Acute Glaucoma
Mannitol is essential for acute glaucoma where rapid reduction of intraocular pressure prevents permanent vision loss. The medication draws fluid from the vitreous humor, reducing eye pressure within minutes.
Acute Kidney Injury Prevention
Osmotic diuretics prevent acute kidney injury in high-risk situations, including:
- Rhabdomyolysis
- Massive transfusions
- Contrast agent exposure
Mannitol maintains high urine flow rates and prevents tubular obstruction, protecting renal function.
Other Clinical Uses
These agents are used in severe hyperkalemia where rapid potassium shifts are needed. However, insulin and glucose are typically used first. Sorbitol has fallen out of favor in many institutions due to the risk of hyperglycemia and gastrointestinal complications, particularly in critically ill patients.
The clinical effectiveness of mannitol in acute conditions makes it a cornerstone medication in intensive care units and emergency departments.
Pharmacokinetics and Administration Considerations
Route of Administration
Mannitol is administered exclusively through intravenous infusion. It is not absorbed orally and would cause osmotic diarrhea if given by mouth. This IV-only route is important to remember for clinical practice.
Dosing and Timing
The typical dosing range is 0.25-1 gram per kilogram of body weight. Dose and infusion rate depend on the clinical situation and patient factors:
- Cerebral edema: rapid administration of 0.5-1 g/kg
- Acute kidney injury prevention: lower doses given more slowly
Mannitol achieves peak osmotic effect within 30-60 minutes. Diuretic onset typically occurs within 15-30 minutes. The duration of action ranges from 4-6 hours.
Blood-Brain Barrier Penetration
A critical pharmacokinetic consideration is that mannitol does not cross an intact blood-brain barrier in significant amounts. This is why it effectively draws fluid from brain tissue into the bloodstream. However, in severe brain injury with blood-brain barrier disruption, mannitol efficacy may be reduced.
Renal Excretion and Accumulation Risk
Approximately 80% of a mannitol dose is excreted unchanged in the urine within 24 hours. In patients with renal impairment, mannitol accumulation is a significant concern. Dose adjustment may be necessary.
Sorbitol, when used, follows similar kinetics but carries additional risks. It is metabolized to glucose in the liver, potentially causing hyperglycemia. Understanding these pharmacokinetic principles is essential for predicting drug efficacy, dosing appropriately, and recognizing when adverse effects might occur.
Adverse Effects and Contraindications
Serious Cardiovascular Complications
While osmotic diuretics are effective, they carry significant adverse effects that limit their use to specific situations. The most concerning adverse effect is hypervolemia and pulmonary edema, particularly in patients with heart failure or compromised cardiac function.
The rapid shift of fluid from interstitial spaces into the bloodstream can overwhelm cardiac output. This risk is especially high in elderly patients or those with renal failure.
Electrolyte and Metabolic Disturbances
Electrolyte disturbances are common, including:
- Hyponatremia
- Hypernatremia
- Hyperkalemia shifts
These depend on the type of fluid losses and reabsorption patterns.
Rebound Intracranial Hypertension
Rebound intracranial hypertension can occur if mannitol is used repeatedly without adequate washout. The agent may eventually equilibrate across a damaged blood-brain barrier and paradoxically increase brain osmolarity. This makes dosing intervals critical.
Hyperglycemia is particularly problematic with sorbitol, which is metabolized to glucose. Sorbitol is contraindicated in diabetic patients.
Contraindications and Special Precautions
Contraindications include:
- Established anuria
- Severe dehydration
- Hyperkalemia (due to diuresis worsening hyperkalemia)
- Intracranial hemorrhage from ruptured aneurysm
Acute kidney injury can paradoxically worsen if mannitol is used inappropriately or in dehydrated patients. Avoid osmotic diuretics in patients with known hypersensitivity. Use cautiously in those with cardiac dysfunction, severe electrolyte abnormalities, or compromised renal function.
Careful patient selection and close monitoring of fluid status, electrolytes, and renal function are essential when using these agents.
Comparing Osmotic Diuretics to Other Diuretic Classes
Loop Diuretics: Mechanism and Effectiveness
Loop diuretics like furosemide work by inhibiting the Na-K-2Cl cotransporter in the thick ascending limb. They produce rapid and potent diuresis but require functional kidneys. They can cause severe electrolyte abnormalities.
Thiazide Diuretics: Chronic Management
Thiazide diuretics inhibit the Na-Cl cotransporter in the distal convoluted tubule, producing moderate diuresis. They are commonly used chronically for hypertension but are ineffective in patients with significant renal impairment.
Potassium-Sparing Diuretics: Limited Potency
Potassium-sparing diuretics block aldosterone or epithelial sodium channels, producing mild diuresis while preserving potassium. However, they are too weak for acute conditions.
Osmotic Diuretics: Unique Advantages
Osmotic diuretics are unique because they create an osmotic gradient independent of active transport mechanisms. This makes them effective even in severely compromised renal function. They produce diuresis without inhibiting ion transport directly.
This mechanism means they do not typically cause severe hypokalemia or hyponatremia from active reabsorption inhibition, though electrolyte shifts can still occur. The rapid onset of osmotic diuretics makes them ideal for acute emergencies like cerebral edema. Loop diuretics are better for chronic fluid overload management.
Additionally, osmotic diuretics can reduce electrolyte reabsorption indirectly through accelerated fluid flow. This provides a distinct therapeutic advantage in specific situations. Recognizing these distinctions allows healthcare professionals to select the most appropriate diuretic for each clinical context.