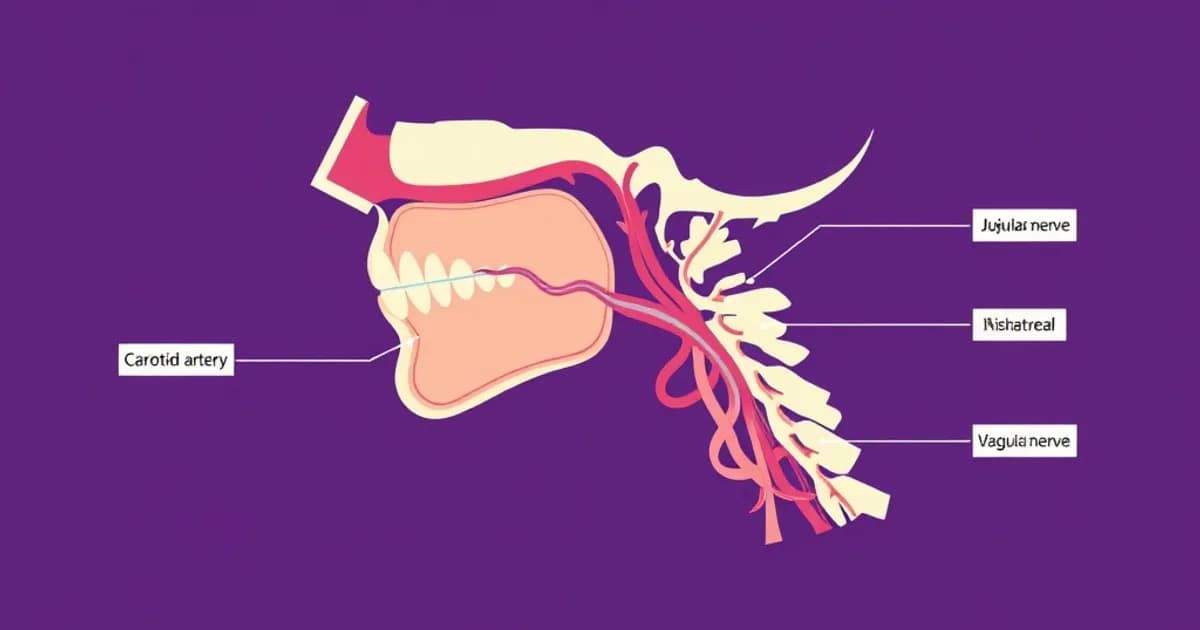
Anatomical Boundaries and Formation of the Carotid Sheath
The carotid sheath is a tubular fascial compartment formed from all three layers of deep cervical fascia. This well-defined compartment creates a distinct anatomical space with major clinical significance.
How the Sheath Forms
The sheath develops from the investing layer (superficial cervical fascia) that splits around the sternocleidomastoid muscle. It combines with the middle cervical fascia (anterior to strap muscles) and the deep cervical fascia (posterior layer). These three fascial layers unite to enclose the vital structures within.
Anatomical Borders and Extent
The sheath extends superiorly to the skull base and inferiorly into the thorax, following the common carotid artery. Laterally, the sternocleidomastoid muscle borders the sheath. Posteriorly, cervical vertebral transverse processes form the boundary. Medially, the pharynx and larynx are adjacent structures.
Clinical Importance
This compartmentalization is critical for understanding complications. Infections or bleeding spread quickly along the sheath's length. Knowledge of sheath anatomy explains how trauma, surgery, or infections progress through the neck. This directly impacts your ability to predict clinical outcomes and surgical complications.
The Carotid Artery: Common, Internal, and External Divisions
The carotid artery system supplies approximately 80 percent of cerebral blood flow, making it essential for brain perfusion. The common carotid artery ascends along the medial sternocleidomastoid border and bifurcates at the C3 vertebral level (superior thyroid cartilage border).
Internal Carotid Artery
The internal carotid artery continues superiorly with minimal neck branching and enters the skull through the carotid canal. This is the clinically most important division because it directly supplies the brain. Lack of initial external branches distinguishes it from the external carotid.
External Carotid Artery and Branches
The external carotid artery immediately branches into multiple vessels. These include the superior thyroid, lingual, facial, occipital, posterior auricular, ascending pharyngeal, and superficial temporal arteries. Understanding these branches helps with imaging and surgical planning.
Specialized Structures at Bifurcation
The carotid sinus monitors blood pressure as a baroreceptor region. The carotid body acts as a chemoreceptor monitoring oxygen levels. These structures are clinically relevant for understanding syncope and cardiovascular reflexes.
Venous Drainage: The Internal Jugular Vein and Its Relationship to the Sheath
The internal jugular vein (IJV) is the largest venous drainage pathway from the brain and head. It begins at the jugular foramen, receiving blood from dural venous sinuses. The IJV descends alongside the internal carotid artery, typically positioned lateral and slightly posterior.
Anatomy and Tributaries
The IJV is larger and more distensible than the carotid artery, allowing it to accommodate increased blood flow during Valsalva maneuvers. Throughout its descent, it receives pharyngeal, lingual, facial, occipital, and superior thyroid veins. These tributaries correspond to external carotid artery branches. The IJV joins the subclavian vein behind the sternocleidomastoid muscle to form the brachiocephalic vein.
Clinical Significance
Damage to the IJV during neck procedures can be catastrophic. Central venous catheterization frequently targets the IJV, making anatomical knowledge essential for safe placement. Understanding IJV anatomy improves your ability to recognize complications on imaging. Knowledge of its position within the sheath guides neck dissections and other surgical interventions.
The Vagus Nerve: Course, Branches, and Clinical Significance
The vagus nerve (cranial nerve X) is the most medial structure within the carotid sheath. It exits the skull through the jugular foramen and descends within the sheath alongside the carotid artery and jugular vein. This nerve serves multiple critical functions throughout the head, neck, and thorax.
Major Nerve Branches
The pharyngeal branch innervates pharyngeal muscles and the pharyngeal plexus, controlling swallowing. The superior laryngeal nerve divides into internal and external branches. The internal branch provides sensory innervation above the vocal cords. The external branch innervates the cricothyroid muscle and controls voice pitch.
The Recurrent Laryngeal Nerve
The recurrent laryngeal nerve has different courses on each side. On the right, it loops under the subclavian artery. On the left, it loops under the aortic arch before ascending to innervate laryngeal muscles and trachea. This nerve is particularly vulnerable during neck surgery due to its course and anatomical relationships.
Surgical Complications
Damage to the vagus nerve or its branches causes serious complications including dysphagia, hoarseness, and voice quality loss. Understanding vagal anatomy helps predict and manage surgical complications. This knowledge is essential for neck procedures like carotid endarterectomy and neck dissections.
Clinical Relevance, Surgical Approaches, and Why Flashcard Study Works
Mastering carotid sheath anatomy is essential for clinical medicine. Carotid endarterectomy removes atherosclerotic plaque and requires precise knowledge of sheath contents. Neck dissections for cancer involve careful identification of adjacent vital structures. Central venous catheterization depends on understanding IJV location and anatomy.
Why Flashcards Work for This Topic
Flashcards break down complex 3D anatomy into testable facts you learn progressively. Rather than memorizing an entire region at once, you master individual components separately: bifurcation level, vagus branches, IJV tributaries, and sheath boundaries. Each flashcard reinforces one key relationship or fact.
Building Long-Term Retention
Spaced repetition ensures long-term retention through multiple exposures over increasing intervals. Active recall during flashcard review forces you to think deeply about anatomical relationships. This method directly improves exam performance and knowledge retention compared to passive study methods.