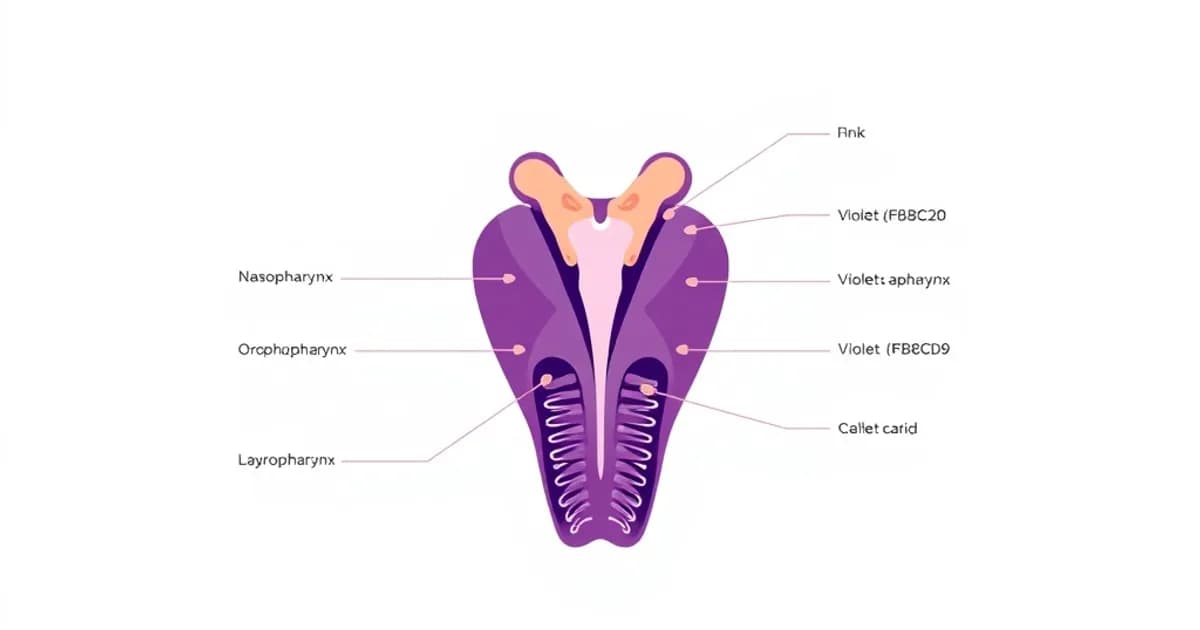
Overview of Pharynx Structure and Divisions
The pharynx is a muscular funnel measuring 12-14 centimeters long. It connects your nasal cavity, oral cavity, and larynx to your esophagus and lungs. Three regions divide the pharynx based on location and function.
The Three Pharyngeal Regions
The nasopharynx lies above your soft palate and behind your nasal cavity. It functions exclusively as an airway. The oropharynx extends from the soft palate down to the epiglottis, where food and air pathways intersect. The laryngopharynx (also called hypopharynx) extends from the epiglottis to the esophagus at the sixth cervical vertebra.
Each region contains distinct structures. The nasopharynx holds the pharyngeal tonsil and Eustachian tube openings. The oropharynx contains the palatine tonsils, tongue taste receptors, and soft palate. The laryngopharynx surrounds the larynx and includes the piriform fossae.
Pharyngeal Wall Layers
The pharyngeal wall consists of four distinct layers. From inside out, these are:
- Mucosa (innermost)
- Submucosa
- Muscular layer
- Buccopharyngeal fascia (outermost)
Clinical Significance of Divisions
Each region has different innervation, blood supply, and susceptibility to disease. This makes targeted study essential for comprehensive knowledge. Understanding these distinctions helps you connect anatomical features to clinical presentations logically.
Pharyngeal Muscles and Their Functions
Pharyngeal muscles organize into two main groups: the constrictors and the elevators. The constrictors propel food during swallowing. The elevators protect your airway and aid in speech.
The Three Pharyngeal Constrictors
These muscles form the primary pharyngeal wall. They work sequentially to move food downward in a process called the pharyngeal reflex. The three constrictors are:
- Superior pharyngeal constrictor: Originates from pterygoid plates, soft palate, and mandible. Innervated by the glossopharyngeal nerve.
- Middle pharyngeal constrictor: Arises from the stylohyoid ligament and hyoid bone. Innervated by the vagus nerve.
- Inferior pharyngeal constrictor: Originates from thyroid and cricoid cartilages. Innervated by the vagus nerve.
These muscles contract in a coordinated, sequential manner that moves the food bolus from the oropharynx into the esophagus.
The Elevator Muscles
The elevator muscles include the stylopharyngeus, palatopharyngeus, and salpingopharyngeus. These raise the pharynx and larynx during swallowing and speech. The stylopharyngeus is uniquely innervated by the glossopharyngeal nerve, while the others receive vagus nerve innervation.
Why This Matters Clinically
Understanding muscle actions and innervation is critical for recognizing swallowing dysfunction. Nerve damage or paralysis produces predictable patterns of weakness. This knowledge helps you diagnose and manage dysphagia and aspiration risk.
Innervation and Blood Supply of the Pharynx
The pharynx receives innervation from multiple cranial nerves working together through the pharyngeal plexus. Understanding these connections predicts how nerve injuries affect function.
Sensory and Motor Innervation
Three cranial nerves innervate the pharynx:
- Trigeminal nerve (CN V): Provides sensory innervation to the nasopharynx and soft palate.
- Glossopharyngeal nerve (CN IX): Provides sensory innervation to the oropharynx and motor fibers to the stylopharyngeus muscle.
- Vagus nerve (CN X): Provides the majority of motor innervation through the pharyngeal branch, innervating all pharyngeal constrictors, elevators, and soft palate muscles.
This overlapping sensory innervation explains why stimulating different pharyngeal areas triggers the gag reflex.
Blood Supply
The ascending pharyngeal artery, a branch of the external carotid artery, provides primary blood supply. It runs along the pharyngeal wall. Additional arteries include:
- Ascending palatine artery
- Dorsal lingual artery
- Maxillary artery branches
Venous drainage returns blood to the internal jugular vein following the arterial pattern. Lymphatic drainage flows to regional lymph nodes including jugulodigastric nodes and deep cervical nodes.
Clinical Applications
Knowledge of nerve anatomy helps predict effects of cranial nerve lesions. Understanding blood supply is essential for surgical approaches and recognizing hemorrhage patterns. Lymphatic knowledge explains how pharyngeal infections spread to regional nodes.
Lymphoid Tissue and the Waldeyer's Ring
The pharynx contains a strategic collection of lymphoid tissue called Waldeyer's ring, which forms a continuous band around the pharynx. This immune structure protects against respiratory and digestive tract pathogens.
Components of Waldeyer's Ring
Waldeyer's ring consists of six main lymphoid structures:
- Pharyngeal tonsil (adenoid) in the nasopharynx
- Palatine tonsils on either side of the oropharynx
- Lingual tonsil at the base of the tongue
- Tubal tonsils near Eustachian tube openings
- Lateral pharyngeal bands
- Additional lymphoid aggregations throughout
Each component contains lymphoid nodules with B and T lymphocytes, macrophages, and dendritic cells. Together they form the mucosa-associated lymphoid tissue (MALT) system.
Immune Function and Age-Related Changes
Waldeyer's ring acts as an immunological defense barrier, filtering pathogens and foreign antigens. The pharyngeal tonsil (adenoid) is most prominent in children and typically shrinks with age. This explains why adenoiditis and obstructive sleep apnea are more common in pediatric populations.
Clinical Significance
Infections in Waldeyer's ring are among the most common infections in primary care. Understanding this anatomy explains symptoms like dysphagia, referred ear pain, and fever during infection. Enlarged structures can cause airway obstruction or chronic ear infections.
Clinical Anatomy and Common Pathological Conditions
Understanding pharyngeal anatomy directly applies to recognizing and managing common clinical conditions. These pathologies demonstrate why detailed anatomical knowledge is essential for clinical practice.
Common Infections and Inflammatory Conditions
Pharyngitis is inflammation of the pharyngeal mucosa, caused by viral or bacterial infection. Symptoms include sore throat, dysphagia, and fever. Tonsillitis is specific infection of the palatine tonsils and often accompanies pharyngitis.
Epiglottitis is inflammation of the epiglottis and represents a medical emergency requiring immediate airway management. Symptoms develop rapidly and can cause airway obstruction.
Structural and Mechanical Conditions
Obstructive sleep apnea frequently involves pharyngeal obstruction due to soft tissue collapse during sleep. Anatomical knowledge helps predict which patients are at risk. Dysphagia (difficulty swallowing) can result from neurological damage affecting pharyngeal nerves, muscular disorders, or mechanical obstruction.
Zenker's diverticulum is an outpouching of the posterior pharyngeal wall. It occurs at a point of anatomical weakness between the inferior pharyngeal constrictor and cricopharyngeus muscle. Patients experience dysphagia and halitosis.
Serious Conditions Requiring Intervention
Pharyngeal malignancy, usually squamous cell carcinoma, often develops in the oropharynx or laryngopharynx. Risk factors include tobacco and alcohol use. Lemierre's syndrome involves septic thrombophlebitis of the internal jugular vein secondary to pharyngeal infection. This rare but serious condition requires immediate antibiotic therapy and often drainage.
Why Anatomy Matters Clinically
Detailed anatomical knowledge predicts symptoms, guides physical examination, and informs treatment decisions. Recognizing anatomical relationships helps you anticipate complications and manage patient safety effectively.