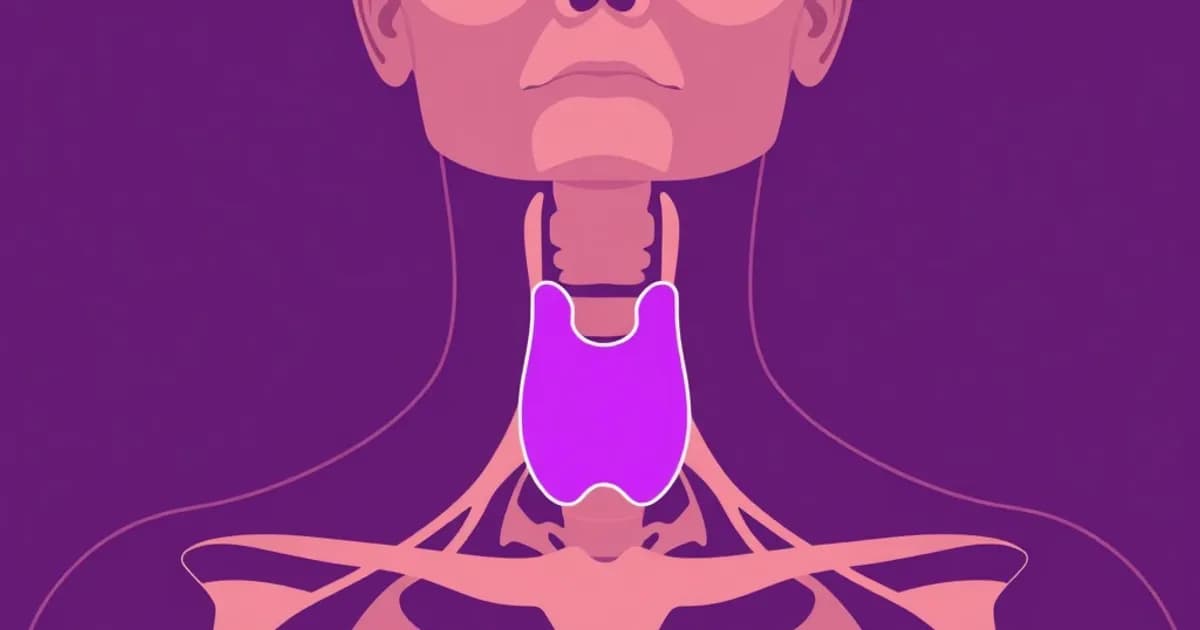
Thyroid Gland Location and Position
Where the Thyroid Sits in Your Neck
The thyroid gland occupies the anterior and anterolateral regions of your lower neck. It sits between the second and sixth cervical vertebrae (C2-C6), just inferior to the thyroid cartilage (also called the Adam's apple).
The gland typically lies at approximately the level of the first and second tracheal rings. This makes it relatively accessible for physical examination through palpation during clinical assessment.
Surface Anatomy Landmarks
The anterior cervical triangle is the key surface anatomy landmark for locating the thyroid. You can identify where it sits by understanding its relationship to two important structures.
Superiorly (toward your head), the hyoid bone marks the upper border. Inferiorly (toward your chest), the sternal notch marks the lower border. The gland spans approximately 4 to 5 centimeters in width and weighs between 15 to 20 grams in healthy adults, making it one of the largest endocrine glands in your body.
Muscular Protection
The thyroid is protected anteriorly by the sternohyoid and sternothyroid muscles. These muscles, part of the infrahyoid muscles, form a protective layer without completely covering the gland. Healthcare providers use palpation techniques to assess the gland for size, nodules, and tenderness during patient evaluations.
Anatomical Structure and Lobes
The Butterfly Shape
The thyroid gland consists of two lateral lobes connected by a central isthmus. This creates its characteristic butterfly or H-shaped appearance when viewed from the front.
Each lateral lobe measures approximately 2 to 3 centimeters in length. They extend from the level of the thyroid cartilage superiorly down to approximately the sixth tracheal ring inferiorly. The isthmus typically overlies the second and third tracheal rings and is generally 1 to 2 centimeters in width.
The Pyramidal Lobe
A pyramidal lobe, a remnant of thyroid embryological development, is present in approximately 30 to 40 percent of individuals. It extends superiorly from the isthmus toward the hyoid bone. This structure helps explain some of the anatomical variations you'll encounter in clinical practice.
Internal Structure and Blood Supply
Internally, the thyroid is composed of microscopic functional units called follicles. Each follicle consists of a single layer of follicular cells surrounding a central cavity filled with colloid.
The thyroid is highly vascularized, receiving blood primarily from the superior and inferior thyroid arteries. Understanding the gland's three-dimensional structure is essential because it explains how thyroid enlargement (goiter) affects nearby structures and why thyroid surgery requires careful anatomical knowledge to avoid damaging the recurrent laryngeal nerve, which runs in the tracheoesophageal groove posteromedial to the thyroid lobes.
Neighboring Anatomical Structures and Relations
Anterior and Lateral Boundaries
The thyroid gland is surrounded by numerous important anatomical structures. Anteriorly, the thyroid is covered by the infrahyoid muscles (sternohyoid, sternothyroid, and sometimes thyrohyoid muscles), the platysma muscle, and skin.
The sternocleidomastoid muscle forms the lateral boundary of the anterior cervical triangle where the thyroid lies. This muscle helps define the boundaries of the anatomical space occupied by the gland.
Posterior and Medial Relationships
Posteriorly and medially, each thyroid lobe contacts the trachea and esophagus. These relationships become clinically important if the gland enlarges, as expansion can compress these vital structures and affect breathing or swallowing.
The recurrent laryngeal nerve runs in the tracheoesophageal groove. It is positioned between the trachea and esophagus on the posteromedial aspect of each thyroid lobe. This nerve supplies motor innervation to the laryngeal muscles and is at critical risk during thyroid surgery. Damage to this nerve can result in voice changes or breathing difficulties.
Superior, Inferior, and Lateral Structures
Superiorly, the thyroid relates to the larynx and hyoid bone. Inferiorly, it may extend into the superior mediastinum, the space in your chest above the heart.
The thyroid contacts the carotid sheath laterally, which contains the common carotid artery, internal jugular vein, and vagus nerve. Understanding these relationships is crucial for clinical practice because thyroid pathology can affect neighboring structures. Surgical approaches must account for these anatomical relationships to minimize complications and preserve function.
Clinical Examination and Palpation Techniques
How to Position the Patient
Examining the thyroid gland clinically requires understanding its anatomical location. The standard technique begins with proper patient positioning.
Have the patient sit with their neck slightly extended, allowing better access to anterior neck structures. This positioning exposes the thyroid without hyperextending the neck uncomfortably.
The Posterior Approach
One effective technique is the posterior approach, where the examiner stands behind the patient. Use both hands to palpate the thyroid lobes from the lateral sides, moving inward toward the midline.
This allows assessment of lobe size, consistency, and the presence of nodules. As the patient swallows, the thyroid gland normally moves upward due to its attachments. This upward movement during swallowing is a normal finding that helps differentiate thyroid tissue from other structures.
What Normal Thyroid Tissue Feels Like
Normal thyroid tissue should feel smooth, soft, and not overly enlarged. Compare the size and consistency of both lobes to ensure symmetry.
Abnormalities that clinicians look for include asymmetry between lobes, nodules (lumpy areas within the gland), tenderness suggesting inflammation, or diffuse enlargement called a goiter. Understanding the precise anatomy helps practitioners differentiate thyroid tissue from other structures like lymph nodes or masses in adjacent tissues.
Why This Skill Matters
Clinical palpation skills are essential for diagnosis of thyroid conditions including hypothyroidism, hyperthyroidism, thyroiditis, and thyroid cancer. Students should practice identifying the thyroid's location through palpation to develop muscle memory and spatial awareness needed for clinical practice.
Embryological Development and Clinical Relevance
How the Thyroid Develops
The thyroid gland develops from endoderm in the floor of the pharynx at approximately the third week of embryonic development. It originates from a pharyngeal outpouching at the base of the tongue.
As the embryo develops, the thyroid descends through the neck, eventually reaching its final position by approximately the seventh week of development. The thyroglossal duct initially connected the developing thyroid to the base of the tongue but normally obliterates and disappears.
Thyroglossal Duct Cysts
When thyroglossal duct remnants persist, they can form thyroglossal duct cysts. This represents the most common congenital neck mass and occurs in approximately 7 percent of the population.
These cysts can become infected or enlarged, requiring surgical removal. Understanding this embryological pathway is clinically important for recognizing this common presentation. Thyroid tissue can sometimes be found ectopically along the midline of the neck, from the base of the tongue down to the normal thyroid location.
The Pyramidal Lobe and Ectopic Tissue
The pyramidal lobe, present in about 30 to 40 percent of individuals, is a remnant of the superior extent of thyroid descent. It represents incomplete obliteration of the thyroglossal duct.
Some individuals may have ectopic thyroid tissue, where thyroid follicles develop outside the normal gland location. The most common site is the base of the tongue, or along the thyroglossal duct path. This anatomical understanding helps clinicians interpret imaging findings and explains unusual presentations of thyroid pathology.