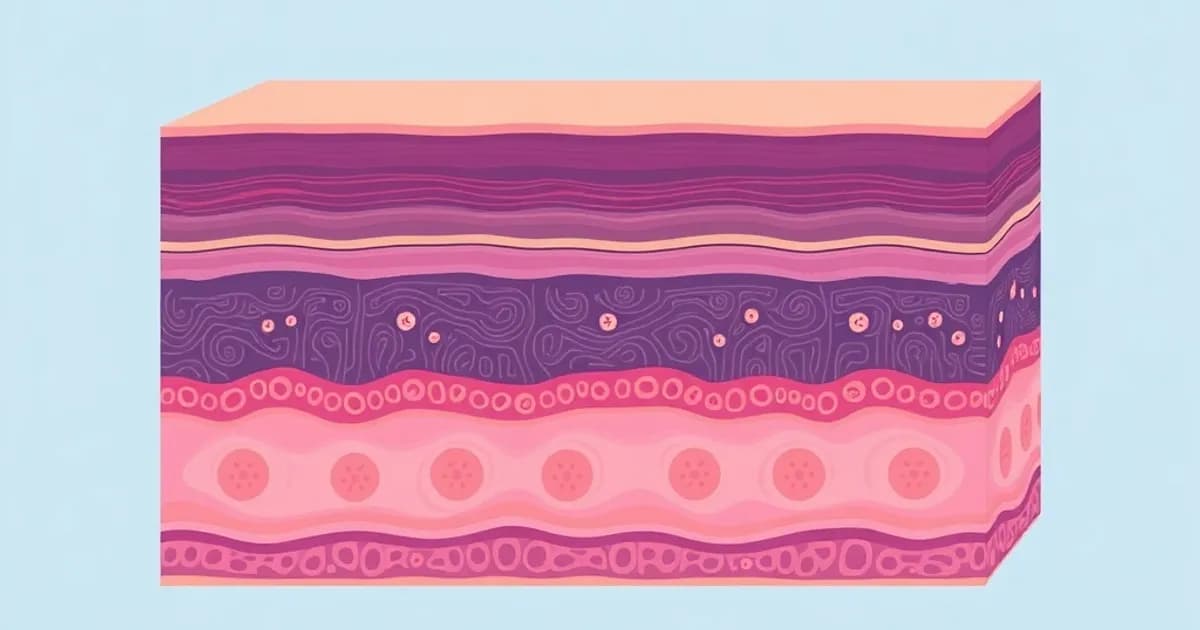
The Five Layers of the Epidermis: Overview and Organization
The epidermis contains five distinct layers arranged from deepest (basal) to most superficial (cornified). From deep to superficial, these are the stratum basale, stratum spinosum, stratum granulosum, stratum lucidum, and stratum corneum. Each layer represents a stage in the keratinocyte lifecycle, from undifferentiated cells in the basal layer to completely dead cells of the corneum.
How Epidermal Layers are Organized
Keratinocytes make up approximately 95% of epidermal cells. The entire epidermis is avascular, meaning it receives nutrients through diffusion from the dermis below. Epidermal thickness varies considerably depending on body location:
- Eyelids: about 0.05 mm
- Palms and soles: up to 1.5 mm
- Most other areas: 0.1 to 0.3 mm
The Keratinization Timeline
The keratinization process (progressive transformation of living cells into dead, protein-filled structures) takes approximately 2 to 4 weeks from the basal layer to shedding at the surface. This continuous replacement system ensures damaged surface cells are regularly removed and replaced with new protective tissue.
Why Layer Organization Matters Clinically
Medical professionals use epidermal layer knowledge to classify skin conditions, predict healing patterns, and determine burn severity. The epidermis's protective function depends entirely on coordinated cell maturation through each successive layer. Deep understanding of these layers connects basic anatomy directly to clinical decision-making.
Stratum Basale: The Germinal Foundation Layer
The stratum basale (also called the basal layer or stratum germinativum) is the deepest epidermal layer and the site of continuous cell division. This single-celled layer sits directly on the basement membrane (basal lamina), which anchors the epidermis to the dermis below.
Cell Types in the Stratum Basale
Stratum basale contains columnar or cuboidal keratinocytes that are actively mitotic, meaning they constantly divide. The layer composition is:
- 90% keratinocytes
- 5% melanocytes
- 3% Langerhans cells
- 2% Merkel cells
Melanocytes produce the pigment melanin, responsible for skin color and UV protection. Merkel cells are mechanoreceptors that sense touch and pressure, creating sensory awareness in the skin.
How Cell Division Works in the Basal Layer
When basal cells divide, one daughter cell remains in the basal layer to maintain the stem cell population. The other is pushed upward into the stratum spinosum and begins the differentiation process. The basal lamina contains hemidesmosomes, specialized cellular junctions creating strong adhesion between epidermis and dermis.
Clinical Significance
Damage to the stratum basale severely impairs skin's regenerative capacity because this layer contains the proliferative cells necessary for replacement. Serious conditions like melanoma or certain forms of epidermolysis bullosa affect the basal layer, disrupting either pigmentation or structural adhesion necessary for skin integrity.
Stratum Spinosum, Stratum Granulosum, and Stratum Lucidum: The Intermediate Layers
These three middle layers represent the transition zone where keratinocytes progressively differentiate and accumulate protective proteins and lipids.
Stratum Spinosum: The Spiny Layer
The stratum spinosum lies directly above the stratum basale and is the thickest epidermal layer. It contains multiple layers of polyhedral keratinocytes connected by desmosomes (specialized junctions giving cells their characteristic spiky appearance under a microscope). As cells move through this layer, they begin expressing keratins and other proteins involved in keratinization.
Stratum Granulosum: The Granular Layer
Located above the spinosum, the stratum granulosum consists of 2 to 4 layers of flattened keratinocytes. These cells contain prominent keratohyalin granules (aggregates of proteins including filaggrin and loricrin). These granules appear as dark spots under light microscopy and represent the transition toward complete keratinization.
The granulosum layer is also the site of lipid synthesis, where keratinocytes produce the lipids that will eventually form the intercellular cement holding cornified cells together.
Stratum Lucidum: The Clear Layer
The stratum lucidum (clear layer) is a thin translucent band visible only in thick skin of the palms, soles, and other high-stress areas. This layer consists of 2 to 3 rows of completely flattened keratinocytes that are losing their nuclei and contain densely packed keratin filaments. The lucidum represents the transition zone between nucleated layers below and the completely anucleate stratum corneum above.
In thick skin, this layer is prominent and clinically significant. In thin skin elsewhere on the body, it may be absent or indistinguishable. These intermediate layers are critical for skin barrier function because cells accumulate the protective proteins and lipids necessary for external protection.
Stratum Corneum: The Protective Barrier
The stratum corneum (horny layer) is the outermost epidermal layer and the primary barrier protecting your body from environmental hazards. Despite being composed entirely of dead cells, it functions as remarkably effective protection.
Structure of the Stratum Corneum
This layer comprises 15 to 20 layers of completely dead, flattened keratinocytes called corneocytes. Think of this layer like a brick wall: corneocytes are the bricks and intercellular lipids are the mortar. Each corneocyte is a flattened, protein-filled cell completely lacking a nucleus and organelles, with a reinforced cell membrane and keratin filaments as its internal structure.
The corneocytes connect to one another through desmosomes that persist even after cell death, maintaining structural integrity. The intercellular lipid matrix consists primarily of ceramides, cholesterol, and free fatty acids in a specific ratio essential for barrier function.
Lipid Barrier Function
The lipid barrier forms a hydrophobic layer that prevents water loss and blocks microbial invasion, making the stratum corneum remarkably effective at protection. This protective mechanism is unique because it works entirely through dead material.
Variation in Thickness Across Body Regions
Stratum corneum thickness varies dramatically by location:
- Eyelids: 10 to 20 micrometers
- Palms and soles: 500 to 600 micrometers
- Most other areas: 50 to 150 micrometers
Thicker regions reflect additional protection needed in high-friction or high-stress areas.
Continuous Shedding and Replacement
Continuous shedding occurs at the surface, with corneocytes sloughed off and replaced by cells moving up from the granulosum layer. This shedding rate is approximately 30,000 to 40,000 cells per minute, meaning the entire stratum corneum is replaced roughly every 2 to 4 weeks. The integrity of the stratum corneum can be assessed clinically, and disruption of this layer leads to increased transepidermal water loss and increased susceptibility to irritants and pathogens.
The Keratinization Process and Clinical Significance
Keratinization is the progressive transformation of living keratinocytes from the basal layer into dead, protein-filled corneocytes of the stratum corneum. This process takes approximately 2 to 4 weeks and is tightly regulated.
Proteins and Molecules Involved in Keratinization
Keratinization involves synthesis of specific proteins including alpha-keratin, filaggrin, involucrin, and loricrin, which provide structural integrity to developing cells. The accumulation of keratins and other proteins gives the stratum corneum its incredible strength and water resistance, allowing skin to withstand mechanical stress and environmental exposure.
Desmosomes and specialized cell junction proteins maintain cell-to-cell adhesion throughout the keratinization process, ensuring cells remain connected even as they die and cornify.
How Skin Conditions Disrupt Keratinization
Many skin conditions and medications affect keratinization:
- Psoriasis accelerates keratinization dramatically, with cells moving from basal layer to surface in only 3 to 7 days, resulting in thick, scaly plaques because cells shed before becoming fully mature
- Retinoids accelerate cell turnover
- Corticosteroids suppress keratinization
- Genetic mutations affecting keratin or filaggrin lead to ichthyosis and atopic dermatitis
Clinical Applications: Burns and Wound Healing
Burns are classified partly by depth. First-degree burns affect only the epidermis. Second-degree burns extend into the dermis. Third-degree burns destroy all epidermal layers including basal layer stem cells.
Wounds extending only through the epidermis can regenerate completely from surviving basal cells. Damage to the basal layer requires tissue grafting or results in scarring. The keratinization process explains why skin has remarkable self-healing properties for superficial injuries: as long as the basal layer survives, new epidermal cells continuously regenerate to replace damaged tissue.