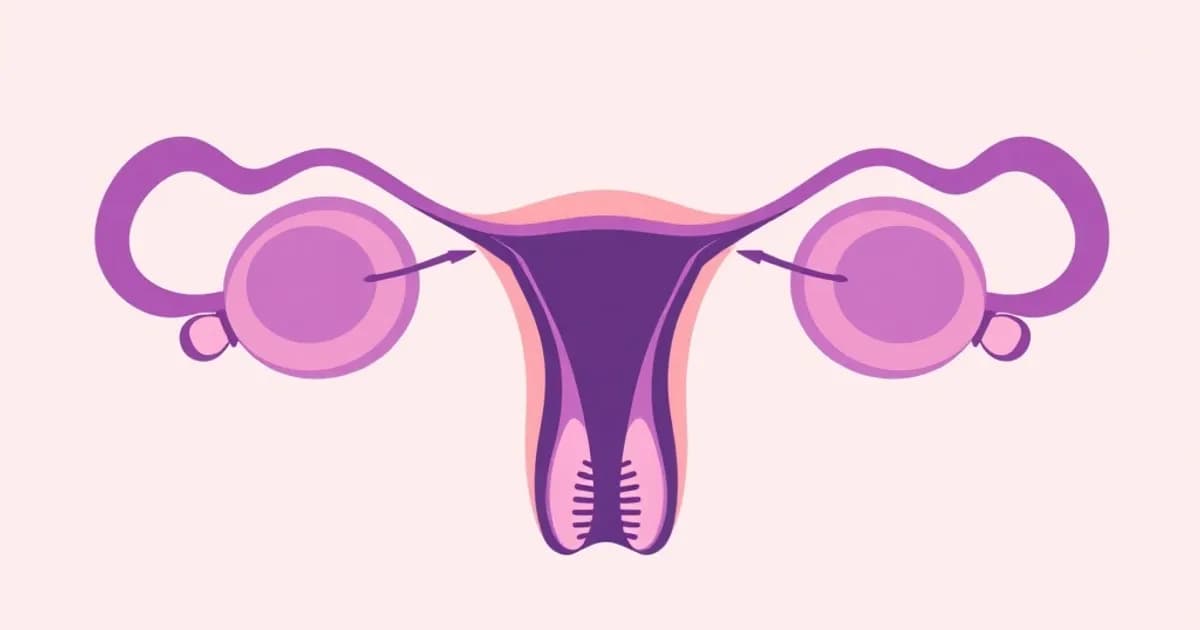
Ovarian Anatomy and Structure
The ovaries are paired, almond-shaped endocrine glands located on either side of the uterus. They measure approximately 3-4 centimeters in length and weigh 6-8 grams each.
Ovarian Regions and Layers
Each ovary has an outer cortex and inner medulla with distinct structural functions. The cortex contains follicles at various development stages. The medulla consists of connective tissue, blood vessels, and nerves.
The ovary's surface is covered by a single layer of cuboidal epithelial cells called the germinal epithelium. Below this lies the tunica albuginea, a dense fibrous connective tissue layer. Unlike many organs, the ovary lacks a peritoneal covering on its surface.
Oocyte Numbers and Development
During fetal development, the ovary contains approximately 1-2 million primary oocytes at birth. This number decreases significantly through atresia (cell death) and ovulation. By menarche, only about 400,000 oocytes remain, with just a few thousand by menopause.
Blood Supply and Innervation
The ovarian artery branches from the abdominal aorta and supplies blood to each ovary. The ovarian vein drains into the inferior vena cava on the right side and the left renal vein on the left side. Understanding ovarian anatomy is fundamental to comprehending follicle development, hormone production, and ovulation.
Follicular Development and the Menstrual Cycle
Follicular development is a continuous process that produces mature eggs ready for fertilization. Understanding this process is essential for mastering reproductive physiology.
Stages of Follicle Development
Ovarian follicles progress through several stages:
- Primordial follicles: A primary oocyte surrounded by a single layer of squamous follicle cells
- Primary follicles: Squamous cells differentiate into cuboidal cells during early growth
- Secondary follicles: Multiple granulosa cell layers form, with fluid accumulating in small spaces called lacunae
- Tertiary (Graafian) follicles: A large fluid-filled antrum surrounds multiple granulosa cell layers, with the oocyte positioned on a stalk called the cumulus oophorus
Hormone-Driven Growth
Follicle-stimulating hormone (FSH) drives these stages during the follicular phase of the menstrual cycle. Theca cells surrounding the follicle produce androgens, which granulosa cells convert to estrogen through the enzyme aromatase.
Rising estrogen levels eventually trigger a surge in luteinizing hormone (LH). This LH surge causes the mature follicle to rupture and release the secondary oocyte, a process called ovulation.
Post-Ovulation Changes
After ovulation, remaining follicular cells transform into the corpus luteum. This temporary gland secretes progesterone and maintains early pregnancy if fertilization occurs. If pregnancy does not occur, the corpus luteum degenerates into the corpus albicans. Understanding this cyclical process is essential for grasping reproductive physiology.
Fallopian Tube Anatomy and Histology
The fallopian tubes, also called oviducts, are muscular ducts extending laterally from the uterus toward the ovaries. Each tube measures approximately 10-12 centimeters in length.
Four Anatomical Regions
Each fallopian tube divides into four distinct sections:
- Intramural portion: The segment within the uterine wall
- Isthmus: A narrow, straight segment
- Ampulla: The widest and most dilated region, primary fertilization site
- Infundibulum: The funnel-shaped terminal end with finger-like projections
The fimbriae are finger-like projections at the infundibulum that surround the ovary and help guide the ovulated egg into the tube.
Wall Structure and Layers
The fallopian tube has four tissue layers:
- Peritoneum: The visceral peritoneal covering
- Muscular layer: Outer longitudinal and inner circular smooth muscle
- Submucosa: Connective tissue layer
- Mucosa: Simple columnar epithelium with specialized cell types
Epithelial Cell Types and Functions
The mucosa contains three main cell types. Ciliated cells beat in coordinated fashion to propel the egg and sperm through the tube. Secretory cells produce fluids that nourish gametes and the early embryo. Peg cells may aid nutrient transport.
The muscular walls contract in a peristaltic manner, assisting in egg movement toward the uterus. Ovarian and uterine arteries provide blood supply. The sympathetic and parasympathetic nervous systems regulate tubal motility and secretion. The mucosa forms intricate folds that are more prominent in the ampulla, providing greater surface area for secretion and sperm capacitation.
Ovulation, Fertilization, and Transport
Ovulation occurs approximately 14 days before the next menstrual period in a typical 28-day cycle. The LH surge, triggered by elevated estrogen, initiates this critical event.
Ovulation and Meiosis
During ovulation, the primary oocyte completes meiosis I, producing a secondary oocyte and the first polar body. The secondary oocyte arrests in metaphase II and completes meiosis only if fertilization occurs.
The follicle ruptures, and the oocyte surrounded by the zona pellucida (transparent protein layer) and corona radiata cells is released. The fimbriae contract and create currents that direct the oocyte into the fallopian tube, though some oocytes may be lost to the abdominal cavity.
Egg Transport and Timing
Once in the tube, the oocyte begins its 3-4 day journey toward the uterus. Fertilization typically occurs in the ampulla within 12-24 hours after ovulation. Sperm travel through the uterus and into the fallopian tubes, guided by chemotactic factors and uterine contractions.
Fertilization Process
Multiple sperm surround the oocyte, but only one successfully penetrates the zona pellucida through acrosomal enzymes. Upon sperm entry, the secondary oocyte completes meiosis II, forming the mature ovum and second polar body.
The male and female pronuclei fuse, completing fertilization and restoring the diploid chromosome number. As the zygote travels down the fallopian tube, it undergoes cleavage divisions, forming a morula and then a blastocyst. Fallopian tube secretions provide essential nutrients during these early developmental stages.
Implantation Timeline
The blastocyst reaches the uterus around day 5-6 post-ovulation and implants into the endometrium approximately 6-10 days after ovulation.
Clinical Significance and Common Pathologies
Understanding ovarian and fallopian tube anatomy is clinically important because pathologies directly impact fertility and reproductive health. Healthcare professionals must recognize these conditions.
Ovarian Conditions
Polycystic ovary syndrome (PCOS) features enlarged ovaries with multiple small cysts, elevated androgen levels, and irregular ovulation. Ovarian cysts can be functional follicles or pathological masses requiring monitoring or surgery. Ovarian torsion is a surgical emergency where the ovary twists on its ligaments, compromising blood supply and causing severe pain.
Fallopian Tube Disorders
Fallopian tube obstruction, caused by scarring from infections, endometriosis, or pelvic inflammatory disease, prevents egg transport and causes infertility. Salpingitis is inflammation of the fallopian tubes, typically caused by sexually transmitted infections or bacteria from the lower reproductive tract.
Pregnancy-Related Conditions
Ectopic pregnancy occurs when a fertilized egg implants in the fallopian tube rather than the uterus. This life-threatening condition requires immediate medical treatment. Tubal ligation is permanent sterilization where the fallopian tubes are surgically cut or blocked.
Other Important Pathologies
Endometriosis, where endometrial tissue grows outside the uterus including on ovaries and tubes, causes pain and infertility. Ovarian cancer originates from epithelial cells covering the ovary and is often diagnosed at advanced stages.
In vitro fertilization (IVF) bypasses blocked tubes by collecting eggs directly from the ovary and fertilizing them in the laboratory. Understanding these conditions requires solid knowledge of normal anatomy and physiology, making comprehensive study essential for healthcare professionals and medical students.