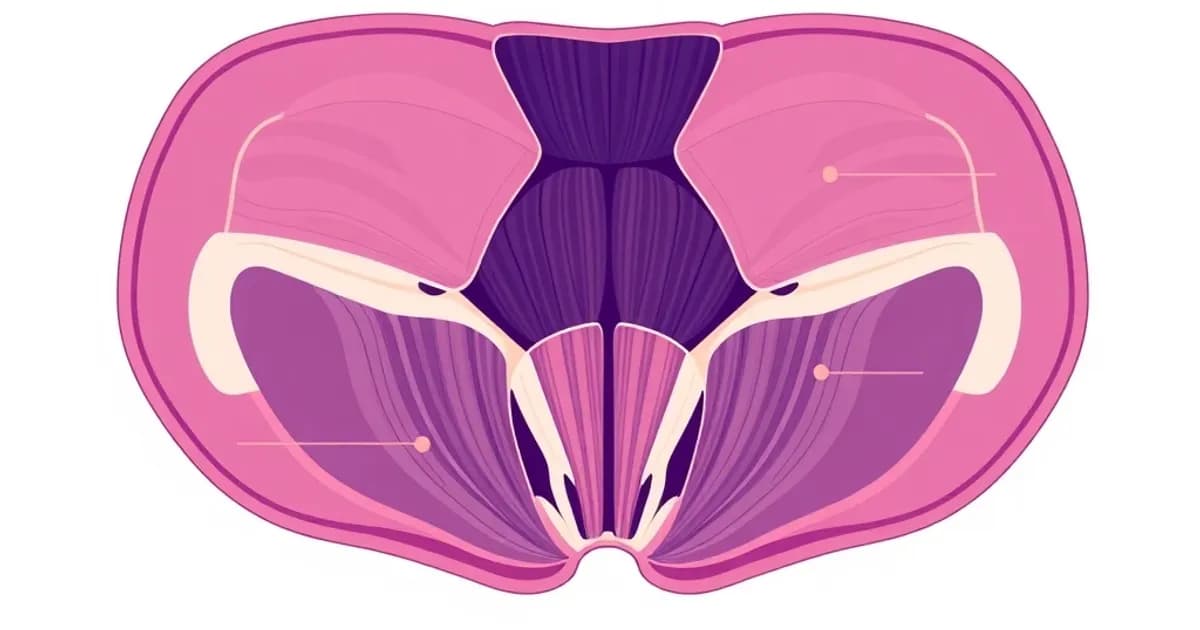
Anatomy and Structure of the Pelvic Floor
The pelvic floor muscles, also called the pelvic diaphragm, consist of three layers of musculature. These form a bowl-shaped structure that supports the pelvic organs.
Main Components
The main components include the levator ani muscles (pubococcygeus, iliococcygeus, and ischiococcygeus) and the coccygeus muscle. Together, these make up approximately 70-80% of the pelvic floor. The levator ani is the largest and most important group, forming a funnel-like structure.
The levator ani extends from the pubic bone anteriorly to the coccyx posteriorly. These muscles attach laterally to the obturator fascia and ischial spines. The puborectalis forms a sling around the rectum that creates the anorectal angle, which is crucial for continence.
Superficial Muscles
The external sphincters sit superficial to the deeper pelvic floor muscles. This includes the external urethral sphincter and external anal sphincter, both voluntary muscles. Understanding the three-dimensional arrangement is essential because these muscles work synergistically to support organs and maintain continence.
Fascia and Support
The pelvic fascia surrounds these muscles and provides structural support. It helps distribute forces throughout the pelvic region. Most students struggle with visualizing this anatomy because it is not easily visible in standard anatomical positions.
Innervation and Nerve Supply
The pelvic floor muscles receive innervation from multiple sources, which is critical for understanding dysfunction. The pudendal nerve, originating from the sacral plexus (S2-S4), is the primary nerve supply for most pelvic floor muscles.
Pudendal Nerve Pathway
The pudendal nerve follows a specific route. It passes through the greater sciatic foramen, around the ischial spine, and through the pudendal canal before branching into terminal divisions. Understanding this pathway is essential because damage at any point can result in pelvic floor dysfunction.
The levator ani muscles receive dual innervation from both the pudendal nerve and direct branches from the sacral plexus. This provides some redundancy in neural supply. Students must memorize the spinal cord levels (S2-S4) and the pathway of the pudendal nerve, as these appear frequently on anatomy exams.
Autonomic Innervation
The pelvic splanchnic nerves (S2-S4) carry parasympathetic fibers that influence bladder and bowel function. These connect through sacral spinal cord segments. Damage to the pudendal nerve during childbirth or prolonged pressure can result in pelvic floor dysfunction.
Autonomic innervation plays a role in reflex mechanisms that control bladder and bowel continence. This represents an important integration point between somatic and autonomic nervous systems.
Functions and Clinical Significance
The pelvic floor muscles perform multiple interconnected functions essential for health and quality of life. These muscles maintain the position of pelvic organs (bladder, uterus or prostate, and rectum) against gravity and increased intra-abdominal pressure.
Supportive and Continence Functions
This supportive function is critical during activities like coughing, sneezing, or exercise. Weakness in these muscles contributes to stress urinary incontinence, particularly in women after childbirth. The continence function involves the external sphincters voluntarily contracting to prevent urine and fecal leakage.
The anorectal angle created by the puborectalis works in coordination with the external anal sphincter to maintain fecal continence. During sexual activity, these muscles contribute to erectile function in males through contraction and relaxation patterns.
Sexual and Stability Functions
These muscles contribute to orgasmic response in both sexes. The muscles also play a role in core stability by providing a muscular floor that stabilizes the spine and pelvis during movement and loading.
Clinical Implications
Clinically, understanding pelvic floor anatomy is essential for recognizing dysfunction presenting as incontinence, pelvic pain, or sexual dysfunction. Childbirth, aging, chronic straining from constipation, and prolonged sitting all weaken these muscles.
Physical therapists use this anatomical knowledge to design pelvic floor rehabilitation programs. Healthcare providers screen for pelvic floor dysfunction because these conditions affect quality of life and are often underreported. Students preparing for clinical practice must understand how anatomical variations and damage patterns correlate with specific symptoms.
Key Muscles and Their Individual Functions
Breaking down the individual muscles within the pelvic floor helps organize knowledge effectively for study. Each muscle has specific origins, insertions, and functional roles.
Major Levator Ani Components
The pubococcygeus, the largest component of the levator ani, primarily supports the pelvic organs. It contracts during activities that increase abdominal pressure. The puborectalis forms a muscular sling around the rectum, creating the anorectal angle of approximately 80-90 degrees when contracted.
This angle is essential for maintaining fecal continence. The iliococcygeus assists in organ support and helps form the lateral walls of the pelvic floor. The ischiococcygeus (coccygeus) extends from the ischial spine to the coccyx and sacrum, providing posterior support.
External Sphincters
The external anal sphincter is a skeletal muscle divided into superficial, intermediate, and deep parts. All parts are under voluntary control, allowing conscious regulation of bowel continence. The external urethral sphincter comprises smooth and striated components, with the striated component under voluntary control via the pudendal nerve.
Superficial Perineal Muscles
The bulbospongiosus muscle in males contracts during ejaculation to propel semen. In females, it surrounds the vaginal opening. The ischiocavernosus assists in erectile function by compressing the corpora cavernosa in males.
Effective Study Organization
Creating organized flashcards for each muscle with its origin, insertion, innervation, and primary action is the most efficient study method. Many students benefit from creating separate cards for deep versus superficial layers to understand functional interactions and clinical examination findings.
Study Strategies and Effective Learning Methods
Mastering pelvic floor anatomy requires strategic study approaches because of its complexity and three-dimensional nature. Flashcards are exceptionally effective for this topic because they force active recall of specific facts like muscle names, spinal cord levels, and functional roles.
Organizing Your Flashcards
Create separate card categories for different types of information. Use one category for muscle anatomy and attachments, one for innervation patterns, and one for functions and clinical correlations. Group related concepts on single cards to build understanding rather than isolated facts.
Pair each muscle with its action and nerve supply on the same card. This approach helps you understand relationships between structures. Color-code your cards by anatomical layer or functional group to aid visual memory.
Visual and Mnemonic Strategies
Visual-spatial learners should supplement cards with anatomical diagrams and three-dimensional models. Use flashcards to test your understanding of what you see in these resources. Create mnemonic devices for remembering the pudendal nerve pathway or the muscles of the levator ani group.
Practice distinguishing between similar structures by creating comparison cards. Examples include different parts of the external anal sphincter or the various branches of the sacral plexus. Use clinical case scenarios on flashcards to link anatomy to practical application.
Spaced Repetition and Integration
Spaced repetition through flashcard apps ensures optimal memory consolidation over time. Combine flashcard study with practical anatomy study by identifying structures on pelvic models or cadaveric specimens. Test yourself on the relationship between anatomical findings and clinical presentations.
For example, connect how pudendal nerve damage correlates with specific types of incontinence. This makes abstract anatomy meaningful and memorable.