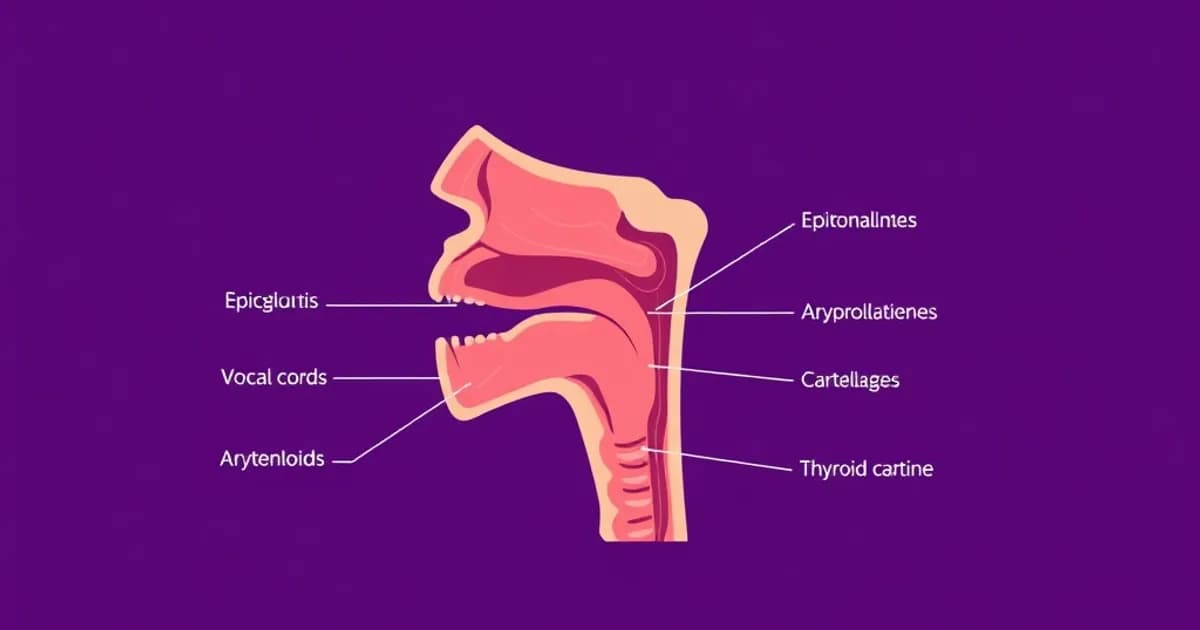
Laryngeal Cartilages: The Structural Foundation
The larynx is supported by nine cartilages organized into unpaired and paired structures. Understanding their relationships is essential because cartilage movements control vocal cord tension, abduction, and adduction.
The Three Unpaired Cartilages
The thyroid cartilage is the largest and most prominent unpaired cartilage, forming the anterior wall and visible as the Adam's apple. It consists of two laminae meeting at approximately 90 degrees in males and 120 degrees in females, which accounts for voice pitch differences.
The cricoid cartilage sits below the thyroid cartilage and is the only complete cartilaginous ring in your entire respiratory tract. This makes it critical for maintaining airway patency. The epiglottis is a leaf-shaped unpaired cartilage that covers the laryngeal inlet during swallowing, preventing food and liquid from entering your airway.
The Three Paired Cartilages
The arytenoid cartilages sit atop the cricoid cartilage as pyramid-shaped structures that control vocal cord movement through muscular attachments. The corniculate cartilages are small horn-shaped structures at each arytenoid apex that serve as ligament attachment points. The cuneiform cartilages are small rod-like structures embedded in the aryepiglottic folds that reinforce the laryngeal inlet.
Each cartilage's position directly affects how your vocal cords move. This relationship between structures is fundamental to both phonation and respiration.
Laryngeal Muscles and Innervation Patterns
Intrinsic laryngeal muscles are classified by their actions: abductors, adductors, and tensors. Learning their innervation patterns is crucial because nerve damage explains specific voice and breathing problems.
Abductors and the Critical Posterior Cricoarytenoid
The posterior cricoarytenoid muscle is the only abductor of the vocal cords and opens your airway. It is innervated by the recurrent laryngeal nerve. When paralyzed, severe breathing difficulties occur because no other muscle can open the vocal cords.
The lateral cricoarytenoid muscles adduct the vocal cords, as do the interarytenoid muscles (transverse and oblique portions). These muscles bring the vocal cords together toward the midline.
Tensors and the Special Cricothyroid
The thyroarytenoid muscle is located within the vocal cord itself and relaxes and shortens the cords, allowing lower pitch phonation. The cricothyroid muscle is unique because the external branch of the superior laryngeal nerve innervates it, not the recurrent laryngeal nerve. This muscle lengthens and tenses the vocal cords, enabling higher pitch production.
Critical Clinical Importance
The recurrent laryngeal nerve innervates all intrinsic muscles except the cricothyroid. This makes recurrent laryngeal nerve injury a major concern in thyroid surgery, cardiothoracic surgery, and conditions affecting the aortic arch.
Unilateral recurrent laryngeal nerve injury causes hoarseness. Bilateral injury causes life-threatening airway obstruction. This innervation pattern explains why specific nerve injuries produce predictable voice changes.
Vocal Cord Anatomy and Phonation Mechanics
Vocal cords are complex structures composed of muscle, ligament, and mucous membrane arranged in layers. These layers vibrate to produce sound during phonation.
Vocal Cord Structure and the Rima Glottidis
Each vocal cord consists of the thyroarytenoid muscle medially and the vocal ligament laterally, covered by stratified squamous epithelium. The space between the vocal cords is called the rima glottidis or glottis, and it changes shape constantly during breathing and phonation.
During inspiration, the posterior cricoarytenoid muscles contract to abduct the arytenoid cartilages. This opens the rima glottidis and allows air passage. During phonation, the lateral cricoarytenoid and interarytenoid muscles adduct the cords, bringing them together so air from your lungs causes vibration.
Microstructure and Mucosal Waves
Vocal cords have a layered microstructure including the epithelium and lamina propria (with superficial, intermediate, and deep layers) plus the vocalis muscle. This layered arrangement allows for mucosal waves that travel from inferior to superior across the vocal cord surface.
Mucosal waves are essential for efficient sound production. Pitch is controlled by varying vocal cord tension through the cricothyroid and thyroarytenoid muscles. Loudness depends on subglottic pressure and the force of vocal cord closure.
Clinical conditions affecting vocal cord mobility, such as nerve injury or muscle dysfunction, directly impact voice quality. Understanding the anatomical basis for these changes is essential for healthcare practice.
Laryngeal Inlet, Spaces, and Clinical Landmarks
The laryngeal inlet and surrounding spaces have precise anatomical relationships that matter for clinical procedures and preventing aspiration. These landmarks guide intubation, endoscopy, and assessment of swallowing dysfunction.
Major Spaces and Structures
The laryngeal inlet is bounded superiorly by the epiglottis, laterally by the aryepiglottic folds, and inferiorly by the false vocal cords. The aryepiglottic folds contain the corniculate and cuneiform cartilages and are important landmarks during endoscopic procedures.
The false vocal cords (also called ventricular folds or vestibular folds) lie superior to the true vocal cords and play a protective role during swallowing. The ventricle of Morgagni is the space between the true and false vocal cords. Its depth varies anatomically, which can affect vocal resonance and quality.
Critical Clinical Landmarks
The anterior commissure is where the vocal cords meet anteriorly and is the most difficult area to visualize during direct laryngoscopy. The posterior commissure is where the vocal cords diverge posteriorly near the arytenoid cartilages.
The piriform recesses are spaces lateral to the larynx where food can lodge if swallowing is impaired, potentially leading to aspiration. The laryngeal vestibule is the space above the false vocal cords and below the epiglottis.
These anatomical relationships explain why aspiration risk is high in patients with laryngeal dysfunction. Endoscopic assessment requires specific technique and knowledge of normal landmarks to safely visualize structures and detect abnormalities.
Laryngeal Ligaments, Membranes, and Blood Supply
Laryngeal ligaments, membranes, and blood supply create a stable yet mobile system that protects your airway while allowing movement during swallowing and speech.
Ligaments and Membranes
The larynx is suspended from the hyoid bone by several important ligaments including the thyrohyoid ligament and membrane, the hyoepiglottic ligament, and the stylohyoid ligament. These structures allow the larynx to move superiorly during swallowing while maintaining stability.
The vocal ligament extends from the thyroid cartilage anteriorly to the arytenoid cartilage posteriorly. It forms the medial edge of the vocal cord. The cricotracheal ligament attaches the cricoid cartilage to the first tracheal ring, creating a mobile but stable connection.
The mucous membrane of the larynx is continuous with the pharynx above and the trachea below. It contains numerous glands that secrete mucus to lubricate the vocal cords. The quadrangular membrane extends between the arytenoid and epiglottis. The conus elasticus (cricovocal membrane) stretches from the cricoid cartilage to the thyroid cartilage and vocal ligament.
Blood Supply and Surgical Implications
The blood supply comes from laryngeal branches of the superior and inferior thyroid arteries, which branch from the external and internal carotid systems respectively. Venous drainage follows a similar pattern, ultimately draining into the internal jugular vein.
The superior laryngeal artery, a branch of the superior thyroid artery, travels with the internal branch of the superior laryngeal nerve. Both structures can be at risk during thyroid surgery if the superior pole vessels are not carefully ligated. Laryngeal hemorrhage can compromise your airway and requires prompt intervention.