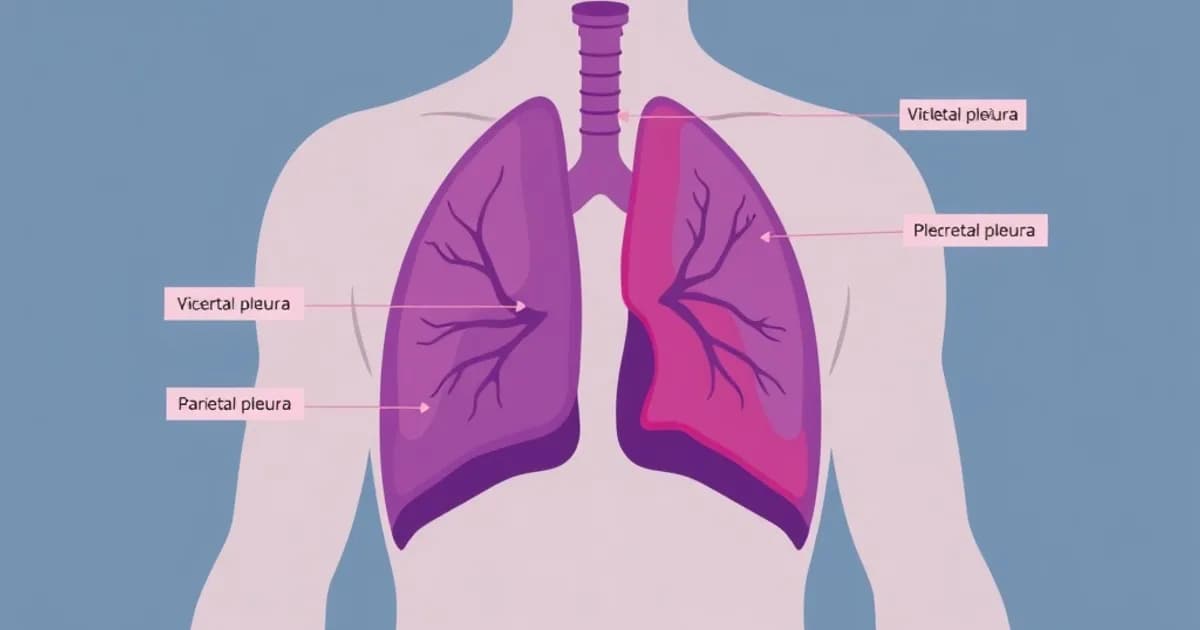
Basic Anatomy of the Pleura
The pleura is a thin, double-layered serous membrane derived from mesoderm. It surrounds each lung and consists of two distinct layers: the visceral pleura and the parietal pleura.
The Visceral and Parietal Layers
The visceral pleura is the inner layer that directly adheres to the lung surface. It covers the entire external lung anatomy including the lobes, fissures, and hilum. This layer is continuous with the parietal pleura at the hilum (where blood vessels, bronchi, and nerves enter and exit).
The parietal pleura is the outer layer lining the inner thoracic wall, mediastinum, and diaphragm. Between these two layers lies the pleural cavity, a potential space containing only a thin film of serous fluid. Under normal conditions, this fluid volume is approximately 10 to 20 microliters.
Subdivisions of the Parietal Pleura
The parietal pleura divides into three regions:
- Costal pleura: Lines the rib cage and intercostal muscles
- Mediastinal pleura: Covers the mediastinal organs
- Diaphragmatic pleura: Lines the superior surface of the diaphragm
Each region has different embryological origins, nerve supplies, and clinical importance. The pleural cavity is completely sealed, creating a negative pressure environment critical for ventilation mechanics.
The serous fluid acts as a lubricant, allowing the visceral and parietal pleura to slide smoothly during respiratory movements. This small but crucial volume enables efficient breathing.
Pleural Reflections and Anatomical Boundaries
Pleural reflections are anatomical boundaries where the visceral pleura becomes continuous with the parietal pleura. These specific lines define the extent of the pleural cavity and are essential landmarks for clinical practice.
Key Anatomical Reflections
At the lung hilum, the visceral pleura becomes continuous with the parietal pleura. This boundary is marked by the pulmonary ligament, a fold of pleura extending inferiorly from the hilum.
The costodiaphragmatic recess (or sulcus) is where the costal pleura reflects onto the diaphragmatic pleura. The inferior boundary varies by location:
- Right side: rib 8 (midclavicular line), rib 10 (midaxillary line), rib 12 (vertebral column)
- Left side: Slightly higher due to cardiac occupation
The costomediastinal recess is where the costal and mediastinal pleura meet anteriorly and medially.
Clinical Importance
These reflections are clinically significant because they define the pleural extent and serve as landmarks for:
- Physical examination
- Imaging interpretation
- Clinical procedures like thoracentesis and chest tube placement
The pleural surface extends from the thoracic inlet (where it rises above the clavicle at the lung apex) down to the costodiaphragmatic recess. The total pleural surface area is approximately 0.6 square meters, highlighting its important role in fluid and gas exchange.
Innervation and Blood Supply of the Pleura
The innervation of the pleura is crucial for understanding both normal physiology and pain patterns in disease. The pleura receives two distinct types of nerve supply.
Visceral Pleural Innervation
The visceral pleura receives visceral afferent fibers that accompany bronchial and pulmonary vessels. These fibers handle mechanoreception and chemoreception but are notably insensitive to pain. This explains why visceral pleural disease often produces minimal discomfort or only referred pain.
Parietal Pleural Innervation
The parietal pleura receives somatic innervation, making it extremely sensitive to pain. Different regions have distinct nerve supplies:
- Costal pleura: Intercostal nerves
- Mediastinal pleura: Phrenic nerves and sympathetic fibers
- Diaphragmatic pleura: Phrenic nerve (from cervical spinal nerves C3 through C5)
Parietal pleural irritation causes sharp, well-localized pleuritic chest pain that worsens with breathing and movement. Irritation of the diaphragmatic pleura can produce referred shoulder pain (called Kehr sign), a clinically important phenomenon.
Blood Supply
The pleura receives blood from systemic arteries:
- Costal pleura: Intercostal arteries
- Mediastinal pleura: Thoracic aorta branches and internal mammary artery
- Diaphragmatic pleura: Phrenic and musculophrenic arteries
- Visceral pleura: Bronchial arteries
Pleural Fluid Dynamics and Clinical Significance
The pleural fluid serves multiple critical functions including lubrication, nutrition, and immune defense. Under normal conditions, approximately 0.1 to 0.2 mL per kilogram of body weight is present (roughly 10 to 20 mL in adults).
Fluid Production and Reabsorption
This thin film of fluid enables smooth movement during respiration. The pleural fluid is produced by capillaries in the parietal pleura and reabsorbed primarily through lymphatic vessels in the parietal pleura and mediastinal pleura.
Fluid dynamics are governed by Starling's forces, which balance:
- Hydrostatic pressure
- Colloid osmotic pressure
- Pleural membrane permeability
Under normal conditions, a delicate balance exists between production and reabsorption. When this balance is disrupted through increased production or decreased reabsorption, pleural effusion develops.
Normal Pleural Fluid Composition
Normal pleural fluid is similar to plasma but with lower protein concentration (typically less than 2 grams per deciliter). Understanding this composition is essential for clinical diagnosis.
Transudate vs Exudate Classification
The Light criteria compare pleural fluid protein and lactate dehydrogenase levels to serum levels. This distinction is crucial:
- Transudates: Suggest systemic disease like heart failure or cirrhosis
- Exudates: Suggest local pleural or pulmonary pathology
Proper classification guides appropriate diagnostic workup and treatment decisions.
Clinical Conditions and Pathophysiology of Pleural Disease
Pleural disease encompasses a wide range of conditions affecting the pleura or pleural cavity. Each has distinct anatomical and physiological mechanisms.
Common Pleural Conditions
Pleural effusion is abnormal fluid accumulation in the pleural cavity. Common causes include:
- Congestive heart failure
- Pneumonia
- Malignancy
- Pulmonary embolism
- Cirrhosis
Pneumothorax occurs when air enters the pleural cavity, disrupting the negative pressure that keeps the lung expanded. A tension pneumothorax is life-threatening, where a one-way valve mechanism allows air entry but not escape, progressively increasing intrapleural pressure and compressing mediastinal structures.
Pleural thickening can result from inflammation, infection, or malignancy. Chronic pleuritis can lead to adhesions between visceral and parietal pleura.
Infectious and Hemorrhagic Conditions
Empyema is a bacterial infection of the pleural cavity creating an exudative effusion. If untreated, it can lead to loculation and fibrous organization.
Hemothorax occurs when blood accumulates in the pleural cavity, often from trauma or bleeding disorders.
Chylothorax results from lymphatic obstruction or rupture, leading to chyle accumulation in the pleural space.
Malignant Conditions
Mesothelioma is a malignant tumor of the pleura associated with asbestos exposure. Understanding the anatomical basis of these conditions helps explain symptoms such as dyspnea, pleuritic chest pain, and hemodynamic compromise. This knowledge guides appropriate diagnostic and therapeutic approaches including imaging studies and invasive procedures.