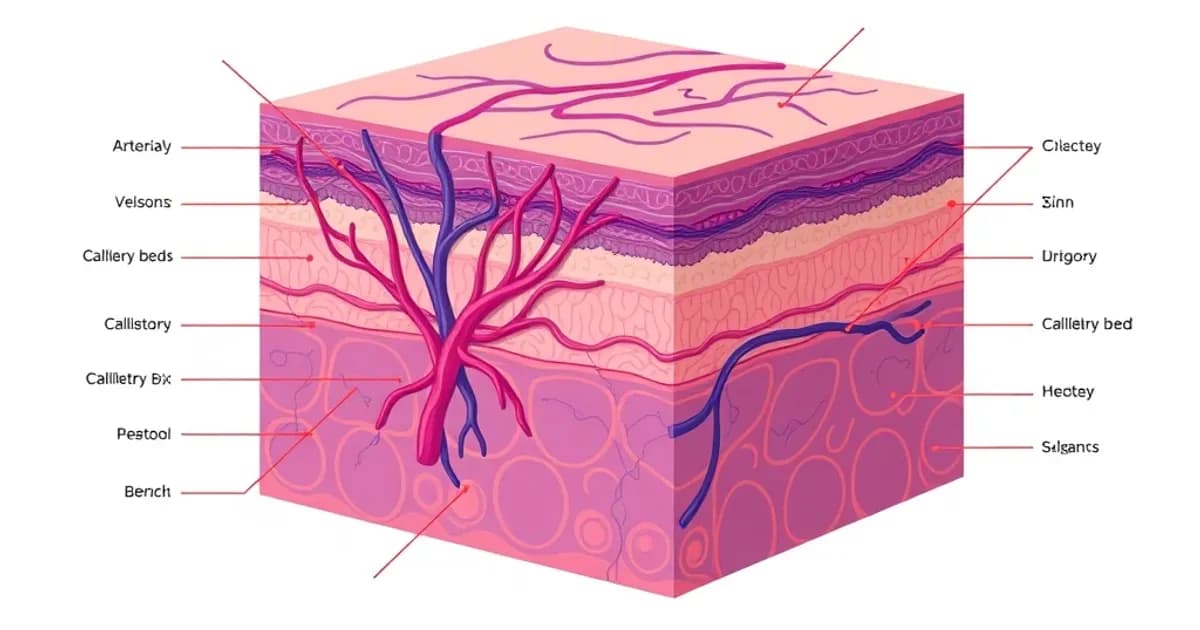
Arterial Supply and Vascular Plexuses
The arterial supply to skin originates from systemic arteries that branch progressively as they approach the integument. Two main types feed the skin: musculocutaneous arteries and direct cutaneous arteries from major vessels.
Three-Level Vascular Organization
As arteries approach the dermis, they form three interconnected vascular plexuses.
- Subcutaneous plexus: Located at the dermis-hypodermis junction. Contains large arteries and arterioles. Serves as the main arterial entry point to skin.
- Dermal plexus (also called subepidermal plexus): Runs horizontally along the dermoepidermal junction. Distributes blood throughout the dermis.
- Papillary plexus: Capillary loops extending into dermal papillae. Provides direct nutrition to the avascular epidermis.
Why Redundancy Matters
These plexuses interconnect extensively, creating redundant blood supply. This is why skin heals well even after significant trauma. If one vessel is damaged, others compensate.
Regional Density Variations
Rich blood supply areas like the face, scalp, and hands have dense, interconnected networks. Limited collateral circulation areas like the shin have sparse backup vessels. This explains why facial wounds heal faster and shin wounds heal slower.
Regional Variations in Cutaneous Blood Supply
Different body regions receive blood from distinct arterial sources. Learning these patterns is critical for surgical planning and predicting complications.
Head and Neck
The external carotid artery branches supply the face with the facial artery, superficial temporal artery, and occipital artery. The scalp receives blood from these same vessels plus the posterior auricular artery and supratrochlear artery. This explains why scalp wounds bleed profusely: multiple large arteries attach firmly to tissue.
Upper Limb
The axillary, brachial, and radial arteries provide cutaneous supply. The radial and ulnar arteries have complementary territories, meaning occlusion of one vessel may not compromise hand perfusion if the other remains patent. This dual system is why hand vascular assessment requires testing both arteries.
Trunk
The intercostal arteries and branches of the abdominal aorta feed the trunk. The superior and inferior epigastric arteries are critical for abdominal wall supply. Surgeons must respect the superior epigastric artery during abdominal incisions to prevent ischemic complications.
Lower Limb
The femoral and popliteal arteries provide most cutaneous supply, with the saphenous vessels offering supplemental coverage. Understanding these patterns helps surgeons design safe flaps and predict ischemic risk.
Venous Drainage and Lymphatic Considerations
Venous drainage parallels the arterial supply but differs in critical ways. Veins are less organized and more variable than arteries, with multiple interconnections allowing alternative routes when one vessel is occluded.
Superficial to Deep Pathway
Superficial dermal veins converge into larger venules, which drain into deeper venous plexuses in the subcutaneous tissue. These plexuses eventually connect to systemic veins returning blood to the heart. The face drains primarily to the internal and external jugular veins. The upper limb uses the cephalic and basilic veins plus deep veins accompanying arteries. The lower limb relies on the saphenous system and deep veins associated with the femoral artery.
Clinical Importance
Venous anatomy explains why facial edema preferentially affects dependent areas. It also clarifies why some regions are prone to venous insufficiency or thrombosis. The valveless nature of facial veins creates special infection risks.
Lymphatic Drainage
The lymphatic system parallels the venous system and is crucial for immune surveillance. Most cutaneous lymph drains to regional lymph nodes before entering systemic circulation. This is why skin infections cause regional lymphadenopathy.
Clinical Correlations and Wound Healing
Understanding cutaneous blood supply explains many clinical phenomena and surgical principles that directly affect patient outcomes.
Surgical Flap Viability
Skin flap survival depends entirely on preserving adequate blood supply. Surgeons use two approaches: random-pattern flaps rely on dermal and subcutaneous plexuses, while axial-pattern flaps depend on specific named arteries. Surgical delay procedures gradually occlude blood vessels to allow new collateral circulation before completing flap elevation.
The angiosome concept represents the three-dimensional territory supplied by a specific artery. Surgeons use this to predict which flaps will survive and which may develop necrosis. Flap complications often result from inadequate understanding of angiosome territories.
Wound Healing Process
Wound healing requires adequate blood supply to deliver oxygen, nutrients, and immune cells while removing metabolic waste. Chronic wounds in areas with compromised circulation, such as venous insufficiency ulcers or diabetic foot ulcers, heal poorly because hypoxia blocks the healing cascade. Understanding vascular insufficiency helps clinicians identify high-risk patients early.
Temperature Regulation and Dermatological Pathology
Increased skin blood flow causes flushing, while vasoconstriction creates pallor in cold exposure. Many dermatological conditions involve vascular pathology: vasculitis affects skin vessels, while vascular malformations like port-wine stains result from abnormal vessel development. Recognizing normal vascular anatomy helps identify pathological changes and predict clinical courses.
Studying Cutaneous Blood Supply Effectively
Mastering cutaneous blood supply requires systematic study combining memorization, visualization, and clinical application. This topic involves many named vessels with distinct origins and territories.
Flashcard Strategy
Create cards testing vessel origins: 'What artery supplies the medial forearm?' Answer: 'Branches of the radial and ulnar arteries.' Make reverse cards: 'What body region does the facial artery supply?' Answer: 'The anterior and lateral face.' Group cards by body region to see patterns rather than memorizing isolated facts.
Visual Learning
Suplement flashcards with anatomical diagrams and 3D visualization. Many students benefit from seeing how vessels branch and anastomose in three dimensions. Practice identifying vessels on anatomical images or cadaver photos when available.
Clinical Application Cards
Create cards linking anatomy to clinical scenarios: 'Why do scalp wounds bleed profusely?' Answer: 'Rich blood supply from multiple arteries with firm tissue attachment.' This deepens understanding beyond rote memorization.
Study Schedule
Use spaced repetition to review challenging cards more frequently than easier ones. Study in multiple daily sessions of 15-20 minutes rather than long cramming sessions. This timing works best for information-dense topics like cutaneous anatomy.